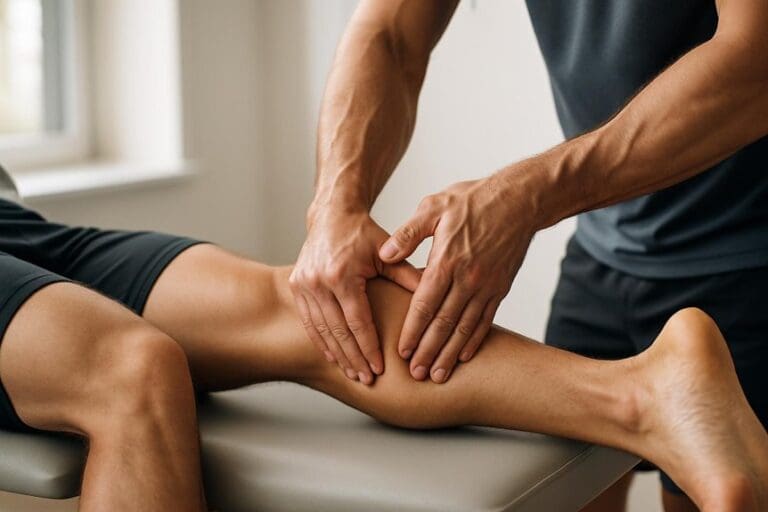
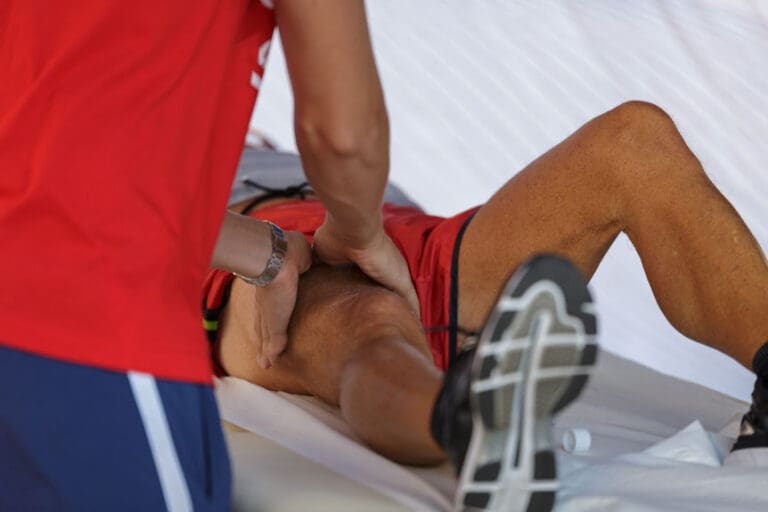
It can help Achilles tendon tightness when the primary driver is calf muscle and fascial stiffness rather than an irritated or injured tendon. Slow, well-dosed pressure and myofascial techniques may reduce guarding, improve tissue glide, and increase short-term ankle dorsiflexion, often making walking feel easier for several hours. Direct tendon pressure is typically conservative, and post-treatment soreness should settle within 24–48 hours. Guidance on red flags, aftercare, and scheduling follows.
Can It Help Achilles Tightness?
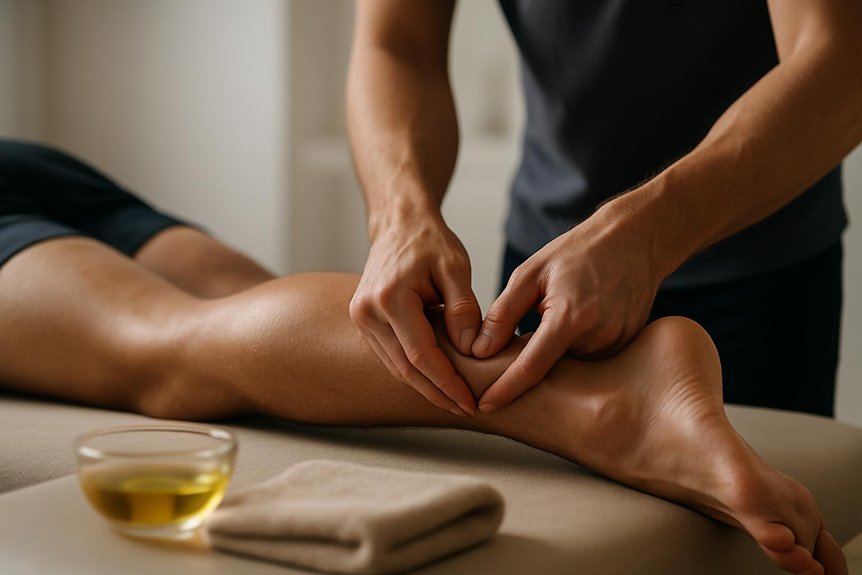
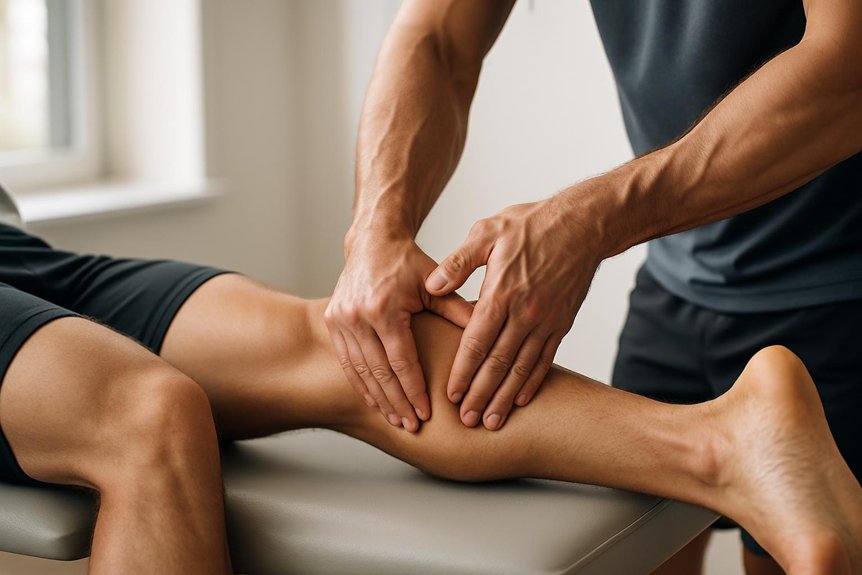
In many cases, intensive tissue massage can help reduce perceived Achilles tightness by addressing contributing soft‑tissue restrictions in the calf (gastrocnemius and soleus), the Achilles tendon’s surrounding fascia, and related lower‑leg musculature. Evidence supports manual therapy for improving short‑term pain and ankle dorsiflexion when calf stiffness is a driver, particularly alongside progressive loading and mobility work. This approach is often used to support the benefits of deep tissue massage by targeting deeper muscle layers and connective tissue restrictions that may contribute to lower‑leg tension.
At Spa & Massage clinics, therapists typically combine slow, specific pressure with myofascial techniques and trigger‑point work, then reassess ankle range and tenderness to keep pressure safe and comfortable. Many clients notice a warmer, looser sensation and easier walking in the hours that follow.
Aftercare usually includes gentle calf stretching, hydration, and avoiding sudden sprinting or hills for 24–48 hours.
When Is Achilles Tightness a Warning Sign?
When should Achilles tightness be treated as more than post‑exercise stiffness? It becomes a warning sign when it is persistent beyond 48–72 hours, increases with ordinary walking, or is paired with morning pain, focal tenderness, swelling, warmth, or creaking sensations along the tendon.
Sudden sharp pain, a “snap” feeling, visible bruising, or weakness when pushing off warrants urgent clinical assessment to exclude a tear.
Tightness with numbness, tingling, fever, or calf swelling/redness should be treated as a same‑day concern.
At Spa & Massage, therapists screen for red flags and keep touch attuned: if symptoms suggest injury, they pause deep work, offer gentle comfort-focused care, and recommend medical review before further treatment.
What Causes Achilles and Calf Tightness in the First Place?
Outside of red‑flag scenarios, Achilles and calf tightness most often reflects a mismatch between tissue load and recovery rather than a single “fault.”
Common drivers include sudden increases in running volume or hill work, reduced ankle dorsiflexion from stiff calf musculature, prolonged sitting or commuting that shortens the gastrocnemius–soleus complex, and footwear choices that alter heel height and tendon strain.
Dehydration, sleep debt, and overall training stress can heighten tone and tenderness, making the area feel “grippy” on first steps.
Previous ankle sprains may change gait and shift load toward the tendon.
In London, lots of walking, stairs, and stop‑start pacing can accumulate.
At Spa & Massage clinics, therapists often hear that stress and bracing through the legs makes calves feel constantly switched on.
Persistent, worsening, or one‑sided symptoms merit assessment.
How Does Intensive Tissue Massage Release Calf–Achilles Tension?
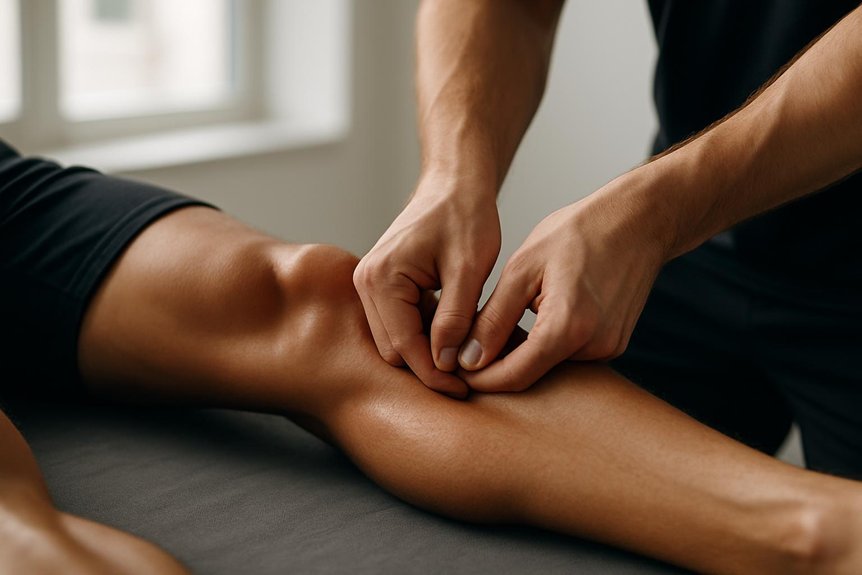
Through targeted, slower-pressure strokes along the gastrocnemius–soleus complex and the Achilles’ surrounding tissues, it helps down‑regulate protective muscle tone, reduce local tenderness, and improve short‑term extensibility so the ankle can move more freely into dorsiflexion.
Mechanistically, sustained, well-dosed pressure can modulate pain sensitivity and calm the nervous system’s guarding response, while focused work around the calf–Achilles interface may improve glide between tissue layers.
At Spa & Massage clinics across London, therapists commonly combine forearm stripping, myofascial release, and gentle cross-fibre work, staying within a “good pain” range and adjusting to each client’s breathing and comfort.
This approach aims to leave the area feeling warmer, softer, and less reactive, supporting more comfortable walking, stair use, and training in the following days.
Intensive Tissue Massage vs Stretching: What Works Best?
How should someone choose between deep therapy massage and stretching for Achilles tightness? Evidence suggests they work best as complements: massage can reduce calf tone and sensitivity, while stretching builds lasting ankle dorsiflexion when done consistently.
If tightness feels protective, sore, or “stuck,” deep tissue work may help create comfortable room for movement; if stiffness is mild and mainly morning-related, a graded stretching programme may suffice.
For tendinopathy, loading and stretching remain primary; massage is supportive, not a stand-alone fix.
At Spa & Massage clinics across London, therapists often pair deep tissue or sports massage with simple home stretches to keep gains between visits.
Any sharp pain, swelling, or sudden weakness warrants clinical assessment before either approach.
What Happens in a Deep Tissue Session for Achilles Tightness?

Typically, a deep tissue session for Achilles tightness begins with a brief clinical intake and movement check to distinguish calf muscle over‑tone from tendon irritability, then progresses to targeted, pressure‑regulated work along the gastrocnemius–soleus complex and adjacent fascial lines while keeping direct force on the Achilles tendon itself conservative.
At Spa & Massage clinics, therapists then warm tissues with slow effleurage, followed by sustained stripping and cross‑fibre techniques to reduce protective tone and improve glide around the posterior compartment.
Pressure is negotiated continuously, aiming for “good pain” without sharpness, heat, or lingering ache.
When appropriate, the ankle is gently moved through dorsiflexion and plantarflexion during contact to refine load tolerance.
The session finishes with calming strokes to settle the nervous system and leave the area feeling safely released.
What Aftercare Keeps Achilles Tightness From Returning?
Often, the difference between short‑lived relief and lasting change in Achilles tightness comes down to aftercare that reduces calf re‑tightening while progressively improving ankle load tolerance.
Spa & Massage therapists advise gentle calf and soleus stretches after warmth, not forcing end‑range. Daily ankle mobility (knee‑to‑wall) supports dorsiflexion without provoking tendon pain.
Load management matters: reduce sudden hill sprints or long walks for 48–72 hours, then reintroduce gradually.
Light self‑massage with clinic‑style aromatherapy oils can calm protective tone and improve comfort, but pressure should stay tolerable.
Hydration and sleep support tissue recovery.
Footwear with adequate heel support and avoiding prolonged tip‑toe postures prevent re‑irritation.
Persistent morning pain, swelling, or sharp tenderness warrants clinical assessment promptly.
How Often Should You Book Deep Therapy Massage for Results?
For clinically meaningful change in Achilles tightness, Spa & Massage typically schedules deep tissue sessions weekly or fortnightly for an initial 3–6 treatments, then adjusts based on objective changes in pain, range of motion, and loading tolerance.
Timing may need to be shorter or longer depending on symptom duration, training volume, tissue irritability, and concurrent rehabilitation such as calf strengthening and mobility work.
To maintain long-term results, most clients shift to periodic maintenance (often every 4–8 weeks) alongside consistent home exercises and activity modifications recommended by the therapist.
Ideal Session Frequency
In many cases, meaningful improvements in Achilles tightness require a structured course of deep therapy massage rather than isolated sessions.
Spa & Massage typically recommends starting with one session weekly for 3–4 weeks to reduce calf and tendon-adjacent myofascial tone and improve glide. If symptoms ease and post-treatment soreness settles within 24–48 hours, sessions can shift to every 10–14 days for another 2–4 visits to consolidate change.
For maintenance, many clients book every 3–6 weeks, particularly during higher training loads or prolonged standing. Each appointment should feel firm yet safe, with pressure adjusted to keep pain below a tolerable threshold and allow relaxation.
Between sessions, the clinics’ therapists advise hydration and gentle ankle mobility on treated days.
Factors That Change Timing
Session frequency provides a useful starting framework, yet the ideal timing between deep therapy massage appointments for Achilles tightness varies with individual risk and recovery factors.
Higher pain sensitivity, recent load spikes (new running, hill work), and morning stiffness that lingers can justify wider spacing to prevent post-treatment flare. Conversely, chronic tightness with low irritability may tolerate closer sessions when paired with progressive calf loading.
Tissue response matters: soreness beyond 24–48 hours, bruising, or increased stiffness suggests the next appointment should be delayed.
Comorbidities (diabetes, anticoagulant use, tendon rupture history) require cautious scheduling and lighter pressure.
At Spa & Massage clinics across London, therapists reassess tenderness, range, and gait each visit, then adjust timing to support safe, steady recovery.
Maintaining Long-Term Results
Beyond the initial improvement phase, maintaining long-term relief from Achilles tightness typically requires a lower, consistency-based booking cadence—often one deep therapy massage every 3–6 weeks—adjusted to symptom return, training load, and post-treatment recovery.
At Spa & Massage, therapists reassess calf–soleus tone, ankle dorsiflexion, and tenderness each visit, then refine pressure and pacing to support tendon load tolerance without provoking next-day flare.
If soreness returns within 10–14 days, sessions may temporarily move to every 2–3 weeks; if symptoms stay quiet, spacing can extend to 6–8 weeks.
Results last longest when massage is paired with progressive calf strengthening, gentle daily mobility, and appropriate footwear.
Many clients in London book around key training blocks or travel to stay comfortable, connected, and confident.
Conclusion
It may reduce perceived Achilles tightness by improving calf soft‑tissue compliance, easing myofascial restriction, and supporting short‑term ankle dorsiflexion, but it is not a standalone fix for tendinopathy or load‑related pain. A notable statistic is that Achilles tendinopathy accounts for around 6–18% of running injuries, underscoring how common calf–Achilles overload can be. Best outcomes typically combine massage with graded strengthening, mobility work, and activity modification, plus review if red flags persist.