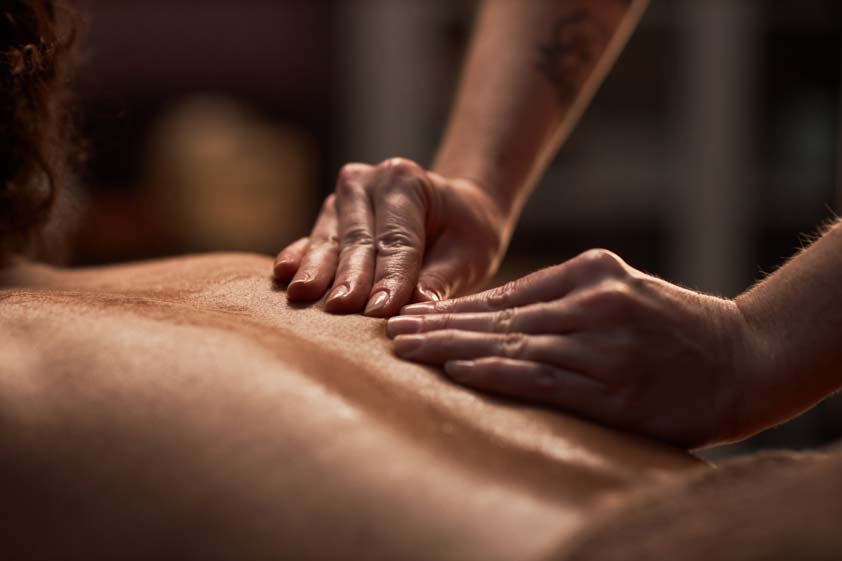
Yes. It can make pain feel worse at first, most often within 24–48 hours, as compressed muscle, fascia, and trigger points are mechanically loaded and sensitized. Slow, deep pressure can create minor microstrain and a short inflammatory response, producing a deep, bruised-like ache rather than sharp pain. Soreness typically improves over 24–72 hours with warmth, hydration, and light movement. Ongoing or escalating symptoms warrant closer guidance in the sections ahead.
Can this Therapy Make Pain Worse at First?

Although it is designed to reduce chronic muscular tension, symptoms can feel temporarily worse in the first 24–48 hours as compressed soft tissue is mechanically loaded and sensitised areas of fascia and trigger points are released.
Microstrain in muscle fibres and connective tissue can stimulate local nociceptors, while increased circulation and lymphatic movement may heighten awareness of previously guarded regions.
Clients often describe a deep, tender ache rather than sharp pain, commonly around the neck, shoulders, hips, and lower back.
At Spa & Massage, therapists pace pressure, follow anatomical landmarks, and check in so intensity stays within a comfortable, intimate “good pain” range.
This response is also consistent with the broader benefits and techniques associated with it.
Gentle hydration, warmth, and light movement usually ease the tenderness as tone normalises.
Sore or Injured After Deep Tissue Massage: Warning Signs
Distinguishing expected post‑treatment tenderness from tissue injury depends on the quality, location, and progression of symptoms in the first 24–72 hours.
Concerning signs include sharp, stabbing pain; a “tearing” sensation; rapidly expanding bruising; marked swelling; heat, redness, or throbbing that localises over one structure rather than spreading through a muscle belly.
Numbness, pins‑and‑needles, new weakness, or pain radiating below the elbow or knee may indicate neural irritation.
Pain that worsens each hour, disrupts sleep, or limits normal joint range can suggest protective spasm or strain.
At Spa & Massage clinics, therapists advise clients to contact the clinic if symptoms feel alarming or unfamiliar, and to seek urgent medical care for fever, severe calf pain, shortness of breath, or sudden loss of function.
What Causes Deep Tissue Soreness?
Once red flags have been ruled out, the remaining post‑massage discomfort is usually explained by normal mechanical and neurological responses to sustained pressure on muscle and connective tissue.
Slow, deep strokes can create micro‑stress within muscle fibres and fascia, prompting a short inflammatory cascade and local fluid shifts that feel like tenderness. Pressure also stimulates nociceptors and alters muscle spindle and Golgi tendon organ signalling, so the nervous system may briefly interpret touch as “sore” while tone recalibrates. Work around trigger points can reproduce referral patterns, leaving a bruised‑like ache without true bruising.
In Spa & Massage clinics, therapists modulate depth, pacing, and breath cues to keep intensity within a client’s safe, connected edge. Hydration and gentle movement can support comfort.
How Long Does Deep Tissue Soreness Last?
Over the first 24–72 hours after an intensive tissue massage, most post-treatment soreness settles as local inflammation resolves and tissue fluid balance normalises. Tenderness is typically felt in compressed muscle bellies, tendon insertions, and along fascial planes that were restricted, especially in the neck, shoulders, lower back, and hips.
In a smaller group, soreness may linger 3–5 days when deeper trigger points were addressed, when baseline stress tone is high, or when the treated area is deconditioned. Discomfort should trend steadily downward; each day should feel looser, warmer, and more pliable rather than sharper. At Spa & Massage, therapists set pressure and pacing to match tissue response, so prolonged pain is uncommon. If soreness escalates, spreads, or limits normal movement beyond a week, reassessment is indicated.
How Can You Ease Soreness After Intensive Tissue Massage?
In the first 24–72 hours post-treatment, soreness after intensive tissue massage can be eased by supporting local circulation, hydration, and nervous-system downregulation while avoiding additional mechanical load on sensitised fibres. Spa & Massage therapists advise gentle walking, diaphragmatic breathing, and warm showers to promote perfusion through treated myofascial layers and reduce protective guarding.
Hydration and electrolyte-balanced fluids support tissue fluid exchange; alcohol is minimised to avoid compounding dehydration. For focal tenderness, a warm compress can relax superficial fascia; brief cool packs may quiet sharper, inflammatory-feeling spots.
Light self-massage with slow strokes and a neutral oil, as used in Spa & Massage clinics, can reassure mechanoreceptors without re-aggravating trigger points. Sleep and magnesium-rich meals assist recovery.
When Should You Avoid Intensive Tissue Massage Next Time?

It should be avoided or postponed when a client has an acute injury or active inflammation, as additional pressure can aggravate irritated muscle fibres, tendons, or joint capsules.
It should also be paused if nerve-related symptoms such as sharp radiating pain, numbness, or tingling are present, since these signs may indicate neural irritation that requires assessment before further manual work.
If post-treatment pain persists beyond 72 hours, Spa & Massage therapists would recommend reassessment and a modified plan rather than repeating the same intensity.
Acute Injury Or Inflammation
After a recent strain, sprain, or flare-up, deep tissue work is typically contraindicated while acute inflammation is present, because high-pressure techniques can aggravate damaged muscle fibres, irritated tendons, inflamed bursae, or joint capsules and may increase swelling, bruising, and pain.
In this phase, tissues are heat-sensitive and chemically irritable; heavy compression may prolong healing and leave a client feeling tender, guarded, and less connected to the area.
At Spa & Massage, therapists screen for redness, warmth, sharp pain, and reduced range of motion, then recommend gentler options such as lymphatic-style strokes, light aromatherapy massage, or careful positioning to support comfort.
Clients are advised to rest, elevate, and use cold therapy, and to rebook deep tissue once acute symptoms settle.
Nerve Pain Or Numbness
Noticing nerve pain, tingling, or numbness during or following a deep tissue session should be treated as a caution sign rather than “normal soreness.”
These symptoms can indicate irritation or compression of peripheral nerves (for example, where a nerve passes between muscles or beneath fascia) or heightened sensitivity from an underlying cervical or lumbar nerve root issue.
At Spa & Massage, therapists would avoid repeating deep, sustained pressure over high-risk areas such as the ulnar groove at the elbow, the fibular head near the knee, the carpal tunnel, or the anterior hip where the femoral nerve and vessels travel.
If sensations radiate, feel electric, or create weakness, the client should request lighter work, stop treatment, and seek clinical assessment.
Future sessions should prioritise gentle, nerve-sparing techniques and precise communication.
Symptoms Last Beyond 72 Hours
When post-treatment soreness, bruising, or restricted range of motion persists beyond 72 hours, it suggests the applied load exceeded the tissue’s recovery capacity and may reflect ongoing inflammation or microtrauma within muscle fibres, fascia, or periosteal-sensitive areas.
In this scenario, deep pressure should be avoided next time until pain settles and movement normalises. Spa & Massage therapists advise booking a reassessment rather than repeating intensity, as persistent tenderness can indicate irritated trigger points, strained tendon insertions, or sensitised nerves.
Clients should pause if sleep is disrupted, swelling increases, or everyday tasks provoke sharp pain.
Gentle heat, hydration, and light mobility may support circulation without reloading tissue.
At the next visit, lighter techniques or sports massage pacing can be used, with clear consent and continual pressure feedback.
Conclusion
It can transiently intensify pain as myofascial adhesions and trigger points are mechanically loaded, provoking localized inflammation and delayed-onset muscle soreness. In one survey, ~10% of massage clients reported discomfort lasting longer than 48 hours, underscoring the importance of pressure titration and screening for acute injury or systemic conditions. When post-treatment tenderness remains diffuse, improves with hydration and gentle movement, and declines within 24–72 hours, it is typically adaptive; escalating focal pain warrants modification or clinical review.