It may help ease lower back pain by calming the nervous system, reducing stress-related muscle guarding, and modulating pain perception, which can support short-term relief and better sleep. It is most suitable for non-specific, mild-to-moderate back discomfort linked to tension, postural strain, or stress sensitivity, especially when direct back work feels too tender. It should not replace medical assessment for persistent, worsening, or neurologic symptoms. Further details can clarify suitability, points used, and safe next steps.
Can It Help Lower Back Pain?
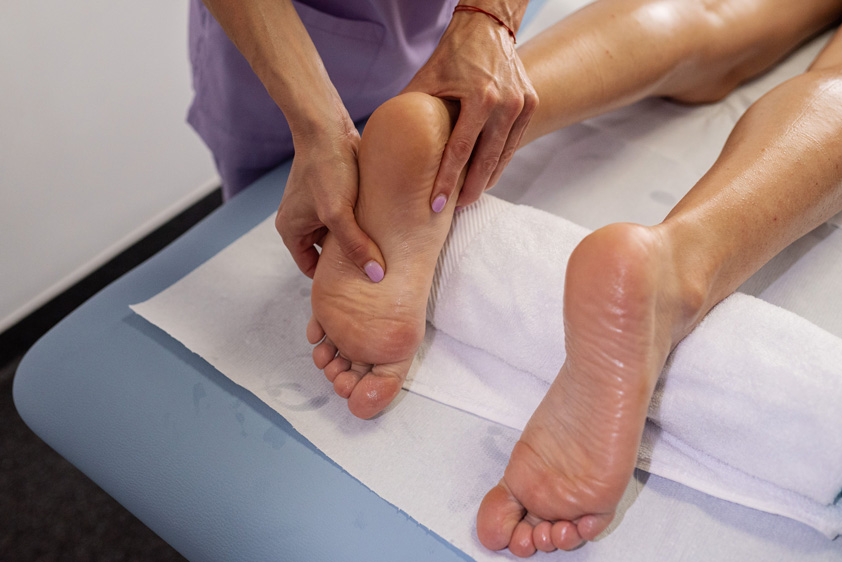
In many cases, it can support the management of lower back pain by modulating pain perception, reducing stress-related muscle tension, and improving relaxation. Evidence suggests it may ease discomfort and improve wellbeing, particularly when pain is non-specific or stress-amplified, though it should not be presented as a stand-alone cure or a substitute for medical assessment. As part of exploring the healing power of reflex therapy, some people use it to encourage whole-body relaxation and support recovery-friendly rest.
At Spa & Massage clinics across London, therapists tailor reflex therapy to the client’s symptoms, sensitivity, and preferences, maintaining clear consent and a calm, private setting. Many clients report feeling soothed, less guarded through the hips and lower back, and better able to rest after sessions. It is often most helpful alongside targeted care, gentle movement, and appropriate clinical guidance, especially when flare-ups feel emotionally draining or sleep-disrupting.
How Does Reflexology Work for Lower Back Pain?
It is often positioned as a supportive option for lower back pain because it targets the nervous system and stress response rather than the lumbar tissues directly.
Pressure to specific foot points is thought to modulate pain processing via afferent nerve input, promoting parasympathetic activity, lowering muscle guarding, and reducing stress-related amplification of pain.
Some people also experience improved circulation and perceived warmth, which can feel soothing during flare-ups.
Clinical evidence is mixed, but many report short-term relief, better sleep, and improved coping.
At Spa & Massage clinics across London, therapists use a gentle-to-firm, consent-led approach, checking comfort throughout and adapting pressure to sensitivity.
It is best framed as an adjunct to medical assessment and active self-care. It can feel calming, grounding, and restorative for clients.
What Types of Lower Back Pain Can It Help?
It may be most helpful for non-specific lower back pain patterns where muscle tension and spasm, heightened stress responses, or postural strain are prominent contributors.
In Spa & Massage clinics across London, therapists commonly see clients whose symptoms relate to prolonged sitting, repetitive activity, or stress-related tightening, and reflex therapy is used as a supportive option to promote relaxation and perceived pain relief.
It is not a substitute for medical assessment, so persistent, worsening, or neurologic symptoms should be appropriately evaluated before focusing on these categories.
Muscle Tension And Spasm
Ease muscular guarding and sudden “gripping” spasms by targeting the nervous system’s pain–tension cycle. It may help when lower back pain is driven by protective muscle tightening around the lumbar spine, sacroiliac area, or hips, often after prolonged sitting, overuse, or a minor strain.
By applying steady, specific pressure to foot zones linked with the lower back and pelvic region, therapists aim to downshift sympathetic arousal, support circulation, and reduce perceived pain, which can allow muscles to release. At Spa & Massage London clinics, reflex therapy is positioned as a gentle option when touch on the back feels too tender; many clients report warmth, softening, and easier movement afterward.
It is best used alongside graded activity and clinical assessment if spasms persist.
Stress-Related Back Pain
Protective muscle tightening is often amplified by stress, poor sleep, and sustained sympathetic “fight-or-flight” activation, which can heighten pain sensitivity and perpetuate low back discomfort even after the initial strain has settled.
In this pattern, the pain is real but maintained by nervous-system arousal, shallow breathing, and reduced restorative recovery.
Reflex therapy may help by supporting a shift toward parasympathetic “rest-and-digest” tone, which is associated with lower perceived pain and improved sleep quality.
At Spa & Massage clinics across London, therapists use calm pacing, consistent pressure, and grounding touch to encourage relaxation, while checking in about comfort and emotional load.
Many clients report warmth, eased guarding, and a feeling of safety that makes movement less threatening.
It is best used alongside sleep hygiene, gentle walking, and stress-management support when needed.
Postural Strain Discomfort
In day-to-day London life, prolonged sitting, habitual slouching, and uneven loading (for example, carrying a bag on one side) can create a predictable pattern of postural strain discomfort in the lower back, marked by tight hips, fatigued paraspinal muscles, and stiffness that typically eases with movement and position changes.
It may help by downshifting the nervous system, reducing perceived muscle tension, and supporting sleep—factors linked with lower pain sensitivity. At Spa & Massage clinics across London, therapists tailor pressure to the client’s comfort and may pair reflex therapy with breathing cues to encourage relaxation without provoking symptoms.
It is most suitable when pain is mechanical, mild-to-moderate, and not associated with leg weakness, numbness, fever, trauma, or bladder/bowel changes.
Which Reflex Therapy Points Are Used for Lower Back Pain?
For reflex therapy sessions targeting lower back pain, therapists typically focus on mapped zones of the feet (and sometimes the hands) that correspond to the lumbar spine and adjacent pelvic structures.
The primary area is the inner edge of each foot from the heel toward the arch, reflecting the lower spinal column; focused, tolerable pressure is applied along this “spine line.”
Additional attention may be given to the heel and lateral ankle region, commonly mapped to the pelvis, sacrum, and sciatic distribution, when symptoms suggest referred discomfort.
Many practitioners also work the arch and midfoot zones often associated with the kidneys, ureters, and bladder, given their relationship to muscle tone and fluid balance.
At Spa & Massage, therapists keep pressure within a comfortable, reassuring range and adapt point selection to the client’s tenderness and pain pattern.
What to Expect From It for Lower Back Pain at Spa & Massage
Typically, a reflex therapy appointment for lower back pain at Spa & Massage begins with a brief clinical-style intake to clarify symptom location, triggers, relevant health history, and goals, so the therapist can tailor pressure, pacing, and point selection to the client’s sensitivity and presentation.
The client remains clothed, resting in a private, tranquil room while the therapist applies measured thumb-and-finger pressure to mapped areas of the feet, adjusting intensity to stay within comfortable, therapeutic limits.
In Spa & Massage clinics, a light, skin-friendly lotion may be used to reduce friction and maintain a grounded, soothing rhythm.
Sensations often include warmth, tenderness, or a deep sense of release; sharp pain is avoided.
Afterward, clients are advised to hydrate, move gently, and note short-term changes in pain, stiffness, sleep, or mood.
Reflexology vs Massage for Lower Back Pain: Which to Choose?
For lower back pain, reflex therapy and massage can both reduce symptoms, but they act through different mechanisms and the strength of evidence varies by pain type and contributing factors.
At Spa & Massage clinics across London, therapists compare expected pain relief based on presentation (e.g., muscle tension, load-related pain, stress-related sensitisation), contraindications, and client preference for direct tissue work versus a foot-based approach.
The choice is then guided by the client’s goals—short-term symptom reduction, improved mobility, or ongoing self-management—often with a tailored plan that may combine both treatments.
Pain Relief Comparison
In clinical practice, choosing between reflex therapy and massage for lower back pain depends on the likely pain drivers (muscle tension, joint stiffness, stress-related sensitisation) and the person’s preferences and tolerances.
Evidence suggests both can reduce pain short-term, mainly via relaxation, improved circulation, and down-regulation of the stress response.
Massage targets local tissues: deep tissue or sports techniques can ease protective spasm and improve comfort with movement, especially when tenderness is clearly muscular.
Reflex therapy works indirectly: focused foot pressure may modulate pain processing and calm the nervous system, which can suit sensitive, touch-averse, or highly stressed clients.
At Spa & Massage, therapists monitor response in-session, adjusting pressure, pace, and positioning to keep treatment soothing yet effective, particularly when the back feels guarded or reactive.
Choosing The Right Treatment
With lower back pain, selecting between reflex therapy and massage is best guided by the person’s dominant symptoms, sensitivity to touch, and the aim of care (local tissue easing versus nervous-system calming).
Massage suits muscular tightness, trigger points, and reduced lumbar mobility; deep tissue or sports techniques can target glutes, hip flexors, and paraspinals while respecting pain limits.
Reflex therapy may fit those who dislike direct back pressure, feel stress-driven pain, or want gentler, whole-body settling through focused foot work and paced breathing.
In Spa & Massage clinics across London, therapists screen red flags, ask about sleep and tenderness, and adapt pressure, positioning, and oils for comfort.
Many clients start with massage for acute stiffness, then add reflex therapy for recovery and calm.
Persistent or radiating pain warrants medical review.
How Many Reflex Therapy Sessions for Lower Back Pain?
Often, meaningful improvement in lower back pain through reflex therapy requires a short course rather than a single session, with the appropriate number depending on symptom duration, baseline pain intensity, functional limitation, and individual response.
For recent, mild discomfort, Spa & Massage therapists commonly suggest 3–4 weekly sessions to assess change in pain, sleep, and ease of movement.
For persistent or recurrent pain, a more structured plan of 6–8 sessions, then spaced maintenance every 3–6 weeks, is often more realistic.
Evidence suggests repeated sessions are more likely to support relaxation, down‑regulate stress responses, and improve pain coping than one‑off visits. Progress should be reviewed after 2–3 sessions; if improvement is limited, the approach can be adjusted.
When It Isn’t Enough: Back Pain Red Flags
At times, lower back pain signals an underlying condition that requires medical assessment rather than continued reflex therapy alone. Spa & Massage advises urgent medical review for red flags: new bowel or bladder changes, saddle numbness, progressive leg weakness, fever, unexplained weight loss, history of cancer, immunosuppression, or severe night pain unrelieved by rest.
Immediate care is also warranted after a fall or accident, or when pain is constant, escalating, or accompanied by significant numbness, tingling, or radiating pain below the knee. Pregnancy-related back pain with bleeding, reduced fetal movement, or severe abdominal pain needs prompt evaluation.
In these situations, reflex therapy may soothe stress but should not delay diagnosis or evidence-based treatment. Appropriate referral can protect long-term function and comfort.
Aftercare Tips After Reflex Therapy for Lower Back Pain
Once serious red flags have been ruled out, aftercare can help consolidate the relaxation and pain-modulating effects many clients experience from reflex therapy for lower back pain.
Spa & Massage therapists advise drinking water, avoiding alcohol, and keeping the body warmly supported for 12–24 hours to reduce post-treatment lightheadedness and muscle guarding.
Gentle walking and slow diaphragmatic breathing can maintain autonomic calming, while prolonged sitting and heavy lifting are best limited that day.
A warm bath or heat pack for 10–15 minutes may ease stiffness; sharp, escalating pain should prompt medical review.
Clients are encouraged to notice sleep, mood, and pain patterns, then book follow-up reflex therapy or a tailored deep tissue or sports massage across the London clinics.
Conclusion
It may offer a gentle, patient‑centred way to support lower back pain by reducing stress, improving perceived comfort, and complementing exercise or manual therapy, though it should not replace clinical assessment. Importantly, low back pain affects about 619 million people worldwide (GBD 2021), underscoring the need for accessible, low‑risk options. Outcomes vary by cause and chronicity, so care is best tailored, monitored, and integrated with evidence‑based management and timely referral when red flags arise.













