It can help reduce sciatica pain when muscle tension in the glutes, hips, or lower back is aggravating the sciatic nerve, often easing a deep ache, burning, or electric pain down one leg. It may improve comfort with walking, sleep, and movement by lowering protective muscle tone and sensitivity. However, during acute flare-ups or suspected nerve root compression, deep pressure can worsen pins and needles, numbness, or weakness and should be avoided. Further guidance below explains safe options.
Sciatica: What It Is and What It Feels Like
Sciatica most commonly refers to pain caused by irritation or compression of the sciatic nerve or its nerve roots in the lower spine. It is a symptom pattern rather than a diagnosis, often linked to disc herniation, spinal stenosis, or muscular entrapment.
People typically describe a deep ache, burning, or electric shock sensation travelling from the buttock down the back of the thigh, sometimes into the calf or foot. Symptoms may include tingling, numbness, or weakness, and can worsen with sitting, coughing, or bending. Pain may be one-sided and fluctuate with posture.
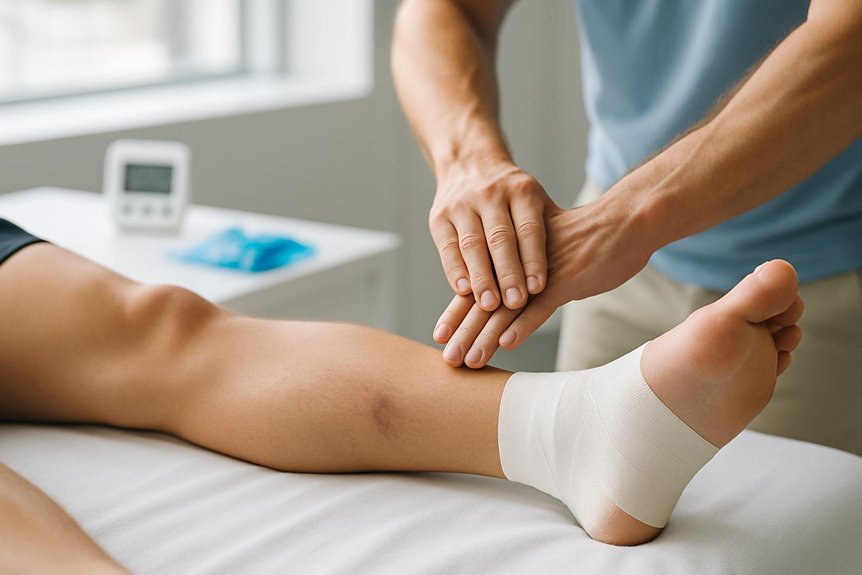
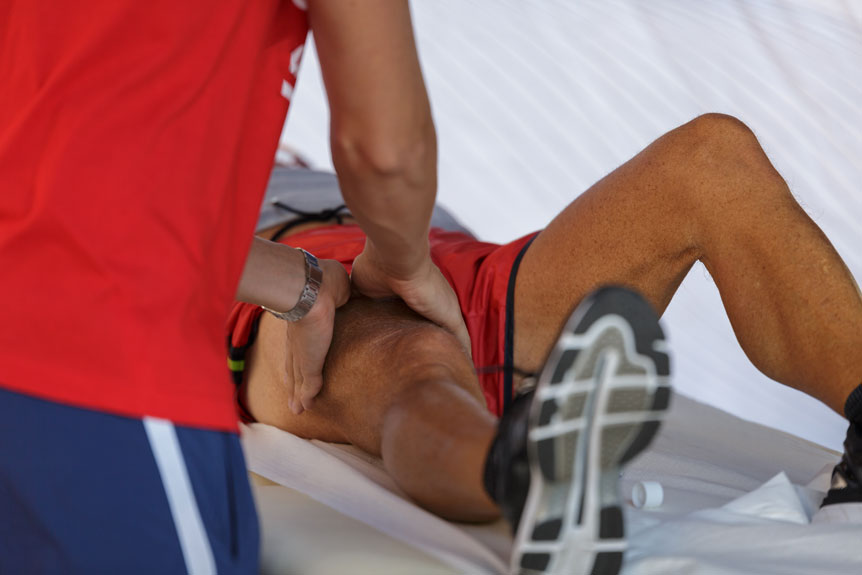
In athletes, sports massage is often used to support recovery and help manage muscle tension that may aggravate symptoms. Red flags include bowel or bladder changes, saddle numbness, fever, or progressive weakness; urgent medical assessment is advised. At Spa & Massage clinics, therapists ask these questions to support safe care.
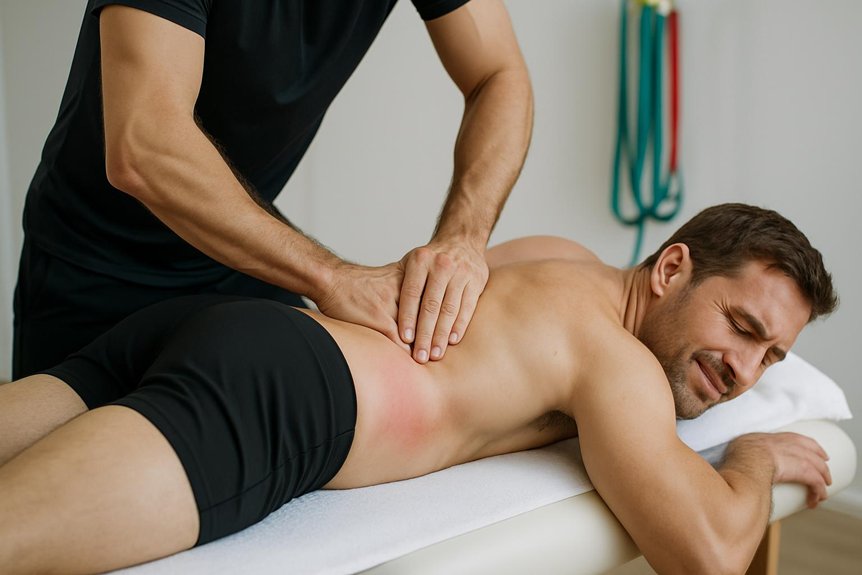
Can Athletic Massage Help Sciatica Pain?
Pain that tracks from the lower back or buttock down the leg often leads people to ask whether athletic massage can reduce symptoms and improve function. Evidence suggests massage may help some people by lowering muscle tone, improving local circulation, and reducing pain sensitivity, particularly when tight gluteal or hip muscles aggravate nerve irritation. It is not a cure for nerve compression, but it can support comfort and movement when used alongside appropriate medical assessment and exercise.
At Spa & Massage clinics across London, therapists assess posture, gait, and tender trigger points, then tailor pressure to the client’s tolerance, keeping treatment calm and consent-led. Many clients report easier walking, improved sleep, and a reassuring sense of being held and listened to.
When It Can Ease Sciatica Symptoms
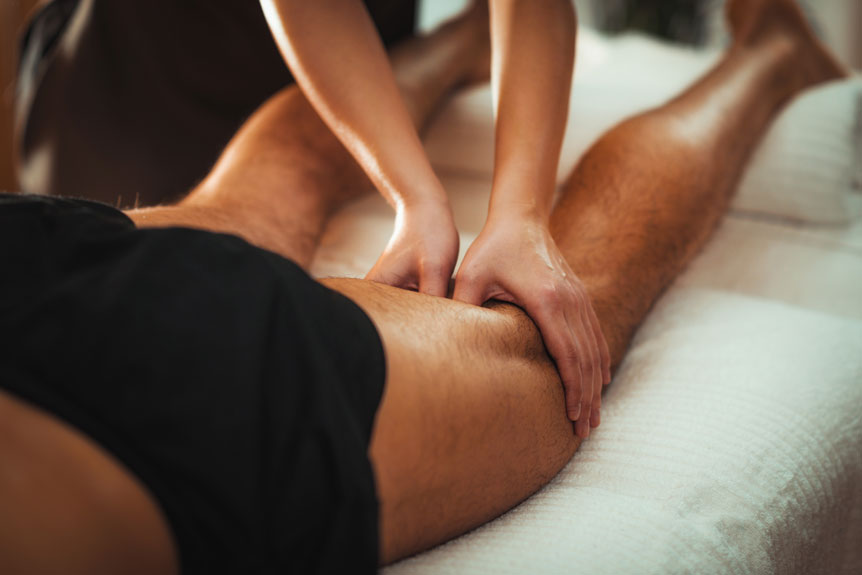
In many cases, athletic massage can ease symptoms when the main driver is soft‑tissue tension rather than ongoing nerve compression—such as tight gluteal, piriformis, hip flexor, or lower‑back muscles that increase sensitivity around the sciatic nerve pathway.
By improving local circulation and reducing muscle guarding, treatment may lessen referred pain, stiffness, and protective spasm, helping movement feel safer and more comfortable.
At Spa & Massage clinics across London, therapists assess posture, hip rotation, and tenderness, then use graded deep‑tissue and myofascial techniques, trigger‑point work, and gentle stretching within the client’s comfort.
Many clients find the most benefit when massage is paired with calm breathing, heat, and a short home routine for glutes and hips.
Relief is often gradual, with sessions spaced to allow tissues to settle.
When Athletic Massage May Make Sciatica Worse
Athletic massage may worsen sciatica during acute flare-ups, particularly when pain is rapidly escalating or accompanied by marked sensitivity along the nerve pathway.
It can also aggravate symptoms when nerve root compression is suspected, as additional mechanical pressure may increase irritation.
At Spa & Massage, therapists screen for these red flags and avoid overly deep techniques, as excessive pressure can provoke pain and inflammation rather than relieve them.
During Acute Flare-Ups
During an acute sciatica flare-up, deep or vigorous manual work may aggravate symptoms by increasing local tissue irritation and provoking protective muscle spasm around the lumbar spine, gluteal region, or along the nerve pathway. Pain can intensify, radiate further, or feel sharper during and after treatment, and sensitised tissues may remain reactive for 24–48 hours.
At Spa & Massage, therapists typically avoid strong pressure and stretching when symptoms are “hot,” focusing instead on comfort-led positioning, slow breath-paced touch, and gentle, indirect work to calm the system. Clients are advised to pause athletic massage if movement pain is escalating, sleep is disrupted, or tingling worsens. In these moments, soothing, supportive care and medical review are prioritised.
With Nerve Root Compression
With true nerve root compression (for example from a lumbar disc herniation or foraminal stenosis), firm athletic massage and aggressive stretching can exacerbate symptoms by increasing mechanical irritation around the affected segment, provoking protective muscle guarding, and amplifying nerve sensitivity—often presenting as escalating radiating leg pain, worsening pins and needles or numbness, or new weakness.
In these cases, symptom behaviour matters more than “tightness”: pain that travels below the knee, progresses after treatment, or is accompanied by strength or sensation changes warrants caution and medical review.
At Spa & Massage, therapists screen for red flags and, when compression is suspected, avoid loading positions and instead use gentle, pain-free work to settle surrounding tissues, support breathing, and encourage comfortable movement.
Any bowel/bladder changes or saddle numbness requires urgent care.
When Technique Is Too Deep
In some cases, an athletic massage technique that is too deep or too sustained can aggravate sciatica by increasing local inflammation, sensitising already-irritated neural tissues, and triggering protective muscle spasm. Symptoms may flare within hours: sharper buttock or leg pain, pins and needles, heightened tenderness, or a feeling of “electric” irritation.
At Spa & Massage, therapists avoid forcing through pain and instead use graded pressure, shorter holds, and careful positioning to keep the lower back and hips feeling safe. If discomfort rises above mild, pressure should be reduced immediately, with emphasis on surrounding muscles rather than the nerve pathway.
Aftercare typically includes gentle walking, hydration, and heat or cold as tolerated. Worsening numbness, weakness, or bladder/bowel changes warrants urgent medical review.
Sciatica Red Flags: When to See a GP or Physio
Sciatic-type pain can sometimes indicate a condition that requires medical assessment rather than massage alone. Red flags include new bladder or bowel changes, saddle numbness, rapidly worsening leg weakness, or severe, unrelenting night pain—these require urgent GP or A&E review.
Immediate medical advice is also recommended after significant trauma, with fever, unexplained weight loss, a history of cancer, or suspected infection.
If pain persists beyond 2–6 weeks, limits walking, or causes progressive pins and needles, a physiotherapy assessment can guide exercise, pacing, and nerve mobility work.
At Spa & Massage clinics across London, therapists screen for these signs, document symptoms, and may pause treatment, advising a GP or physio to keep care safe and coordinated.
Athletic Massage Techniques We Use for Sciatica Relief
For many clients, it provides symptom relief when sciatica is driven by irritated neural tissue alongside overload and tightness in the hip and lower-limb musculature.
At Spa & Massage clinics, therapists use slow, specific deep-tissue strokes to the gluteals, piriformis, hamstrings, and calves to reduce tone and ease protective guarding around the nerve pathway. Trigger-point pressure may be applied to referred-pain hotspots, with client-led pacing and clear consent to keep discomfort therapeutic.
Myofascial release and gentle longitudinal stripping can improve tissue glide, supporting freer hip movement. When tolerated, light nerve-flossing style mobilisations and diaphragm-led breathing are paired to downshift sensitivity.
Sessions finish with soothing effleurage and simple aftercare: warmth, hydration, and gradual return to activity.
What We Assess in a Sciatica-Focused Appointment
How does a therapist determine whether it is appropriate for sciatica-like symptoms? At Spa & Massage, the appointment begins with a detailed history: onset, pain map, pins-and-needles, weakness, sleep disruption, and aggravating movements. Therapists screen for red flags (saddle numbness, bladder/bowel changes, progressive weakness, fever, recent trauma) and refer onward when indicated.
A focused physical assessment follows: posture, gait, lumbar and hip range, neural tension tests, and palpation of the gluteals, piriformis, and paraspinals to distinguish referred pain from nerve irritation. They also consider training load, work ergonomics, and stress, because muscle guarding can amplify symptoms.
Together, therapist and client agree comfort limits, pressure preferences, and a plan prioritising safety and soothing touch.
How Many Massage Sessions for Sciatica?

Often, the number of massage sessions needed for sciatica-like symptoms depends on symptom irritability, duration, functional limits, and the drivers identified during assessment (e.g., gluteal/piriformis guarding, lumbar stiffness, training-load spikes, or prolonged sitting).
At Spa & Massage, many people start with 3–6 sessions over 2–4 weeks to calm protective tone, improve load tolerance, and restore comfortable movement.
More persistent or recurrent presentations may require 6–10 sessions, spaced weekly then tapered as symptoms stabilise.
Session-to-session decisions should be guided by measurable changes: pain intensity, sleep comfort, walking or sitting tolerance, and ease of bending.
If there is no meaningful improvement after 2–3 visits, reassessment is indicated to refine the plan and consider referral for medical evaluation.
Self-Care Between Massage Sessions for Sciatica
Session frequency can help settle sciatica-like symptoms, but day-to-day choices between appointments often determine how well gains hold.
Spa & Massage therapists encourage gentle movement “snacks” every hour: short walks, pain-free hip hinges, and nerve-glide drills only if they feel easing, not sharp.
Heat may relax guarded muscles; brief ice can calm flare-ups—both used for 10–15 minutes with skin protection.
Sleep support matters: side-lying with a pillow between knees or supine with calves elevated often reduces morning irritability.
Hydration and light self-massage to glutes with a ball can ease tenderness, avoiding direct pressure over the nerve.
If new weakness, numbness, or bowel/bladder changes appear, urgent medical review is advised.
Conclusion
It may support sciatica care by soothing secondary soft‑tissue strain, reducing protective spasm, and restoring sensible movement, particularly when symptoms stem from muscular tension and mobility limits. It cannot “cure” nerve compression, and poorly placed pressure may provoke pain, so screening and skilled, symptom‑led techniques matter. With red‑flag awareness and medical guidance when indicated, massage can complement strengthening, stretching, and posture practice—promoting steadier function, safer activity, and more sustainable recovery.