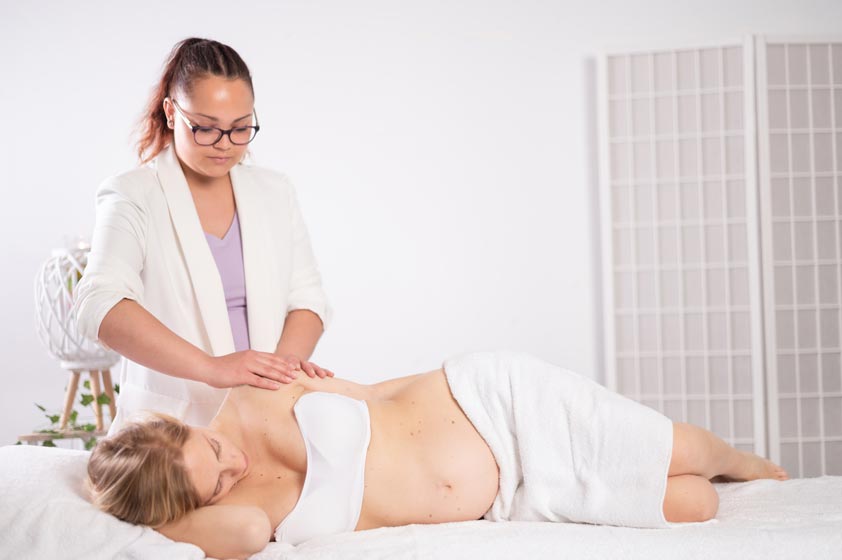
Prenatal massage should be avoided with high‑risk pregnancy, acute complications, or clinician‑advised restrictions, including pre‑eclampsia, placenta praevia, significant bleeding, threatened miscarriage, or preterm labour risk. Cancel the appointment with vaginal bleeding, leaking fluid, severe abdominal or pelvic pain, regular contractions, reduced fetal movement, fever, fainting, chest pain, shortness of breath, sudden severe headache with visual changes, unilateral calf swelling, or rapid facial/hand swelling. Medical clearance is advised for clotting disorders, anticoagulants, uncontrolled hypertension, or recent hospitalisation. Further guidance covers trimester‑specific precautions.
When Should You Avoid Prenatal Massage Completely

As a rule, prenatal massage should be avoided completely when there is a clear medical contraindication or an acute complication in pregnancy. This includes situations where a midwife or obstetrician has advised restriction, or where the pregnancy is classified as high risk and hands-on therapy has not been explicitly cleared. When appropriate and medically cleared, pregnancy massage can support comfort and relaxation for expecting mothers.
At Spa & Massage, therapists require medical approval before treating clients with conditions such as pre-eclampsia, placenta praevia, significant bleeding history, threatened miscarriage, preterm labour risk, uncontrolled hypertension, or serious cardiac, renal, or clotting disorders.
Massage is also deferred after invasive procedures or hospital admissions until the care team confirms stability. When clearance is granted, sessions are adapted: side-lying positioning, gentle pressure, careful avoidance of high-risk areas, and meticulous comfort checks throughout.
Pregnancy Symptoms That Mean Cancel Today
On the day of a scheduled prenatal massage, any symptom suggesting acute pregnancy complication should prompt cancellation and same-day clinical advice.
Red flags include vaginal bleeding, leaking fluid, sudden or severe abdominal/pelvic pain, regular contractions, reduced or absent fetal movements, or new severe headache with visual changes.
Cancel if there is fever, chills, vomiting with dehydration, fainting, chest pain, shortness of breath, unilateral calf swelling/pain, or rapid facial/hand swelling.
New-onset high blood pressure symptoms, persistent right‑upper‑quadrant pain, or seizures require urgent care.
At Spa & Massage, therapists will pause treatment if a client reports these concerns and encourage immediate medical assessment; comfort and closeness are best supported when safety is unquestioned.
Reschedule once symptoms resolve and reassurance is obtained.
When You Need Medical Clearance for Prenatal Massage
Symptoms that warrant cancelling on the day are immediate red flags; a separate question is when prenatal massage may be appropriate but should only proceed with medical clearance. Clearance is typically needed with high-risk pregnancy, history of preterm labour, cervical insufficiency or cerclage, placenta praevia, unexplained vaginal bleeding earlier in pregnancy, pre-eclampsia or uncontrolled hypertension, gestational diabetes requiring medication, clotting disorders or anticoagulants, previous DVT/PE, significant swelling, or heart, kidney, or autoimmune disease.
It is also prudent after recent hospital admission, surgery, or when mobility restrictions are prescribed. At Spa & Massage, therapists request written guidance on positioning, pressure limits, and any areas to avoid, so touch remains soothing, intimate, and clinically safe throughout treatment.
Is Prenatal Massage Safe in Every Trimester?
Across pregnancy, prenatal massage can be safe in every trimester when it is delivered by a pregnancy-trained therapist using trimester-appropriate positioning, pressure, and contraindication screening; however, the risk profile and clinical precautions differ between the first, second, and third trimesters.
In the first trimester, therapists typically use lighter pressure, avoid prolonged heat, and prioritise conservative work given higher baseline nausea, fatigue, and early pregnancy uncertainty.
In the second trimester, side-lying support allows comfortable, intimate relaxation while maintaining neutral spinal alignment and avoiding abdominal compression.
In the third trimester, careful bolstering, shorter prone-avoidant sessions, and vigilance for swelling, hypertension, or thrombotic risk are essential; deep work over calves is avoided when red flags exist.
At Spa & Massage, prenatal massage is adapted session-by-session and stopped if concerning symptoms appear.
Pregnancy-Safe Alternatives to Prenatal Massage
Prenatal massage can be appropriate in any trimester when delivered by a pregnancy-trained therapist with correct positioning and contraindication screening, but some clients will still be advised to postpone hands-on treatment due to symptoms, risk factors, or medical guidance.
Pregnancy-safe alternatives can still support comfort and closeness without deep manual work.
At Spa & Massage, therapists often suggest gentle, non-invasive options: guided breathing for down-regulation, supported side-lying rest with pillows, and heat-free aromatherapy inhalation using pregnancy-appropriate blends rather than abdominal application.
Reflexology may be offered with light pressure and symptom-led pacing when the midwife or GP has no concerns.
Simple home care includes short walks, calf pumps to reduce swelling risk, hydration, and sleep positioning with a pillow between knees.
Any new pain, bleeding, fever, or reduced fetal movement warrants medical review.
Conclusion
Prenatal massage is not universally appropriate; it should be avoided with bleeding, severe abdominal pain, suspected pre‑eclampsia, fever, reduced fetal movements, or other red‑flag symptoms, and deferred in many high‑risk pregnancies until medical clearance is documented. A common objection is that “gentle massage can’t harm,” yet pregnancy complications can evolve rapidly and contraindications are often symptom‑based rather than pressure‑based. Structured screening, trimester‑appropriate positioning, and safer alternatives help reduce risk.