Reflex therapy points for back pain are primarily addressed along the medial edge of each foot on the spinal reflex line, tracing from the hallux (cervical) through the inner arch (thoracic/lumbar) to the inner heel (sacrum/coccyx). Lower-back focus typically includes the medial longitudinal arch and the central-to-inner heel margin, with secondary attention to the plantar heel pad and inner ankle groove. Pressure is applied via thumb-walking or 3–6 second compressions, “strong but not sharp,” with ongoing consent and red-flag screening. Further guidance clarifies mapping, dosing, and referral thresholds.
Reflex Therapy Points for Back Pain: What to Expect

During an initial reflex therapy session for back pain, the client can expect a structured assessment followed by targeted pressure work on mapped foot zones associated with the lumbar, thoracic, and sacral regions. At Spa & Massage clinics, therapists take a brief health history, screen contraindications (e.g., acute inflammation, thrombosis risk, recent fracture), and agree comfort boundaries and pressure preferences.
Technique typically uses thumb-walking, hook-and-backup, and sustained compressions, progressing from lighter palpation to deeper, slow pressure to locate tenderness and tissue congestion. The client remains fully clothed, feet supported, and the room kept warm to encourage parasympathetic downshift. Reflexology is often described in terms of its potential healing power when applied with appropriate mapping and pressure. Communication is continuous, inviting micro-adjustments for intimacy without overstimulation.
Aftercare may include hydration, gentle mobility, and monitoring of transient soreness, with referral guidance if red flags appear.
Reflex Therapy Points Linked to the Back (Foot Map)
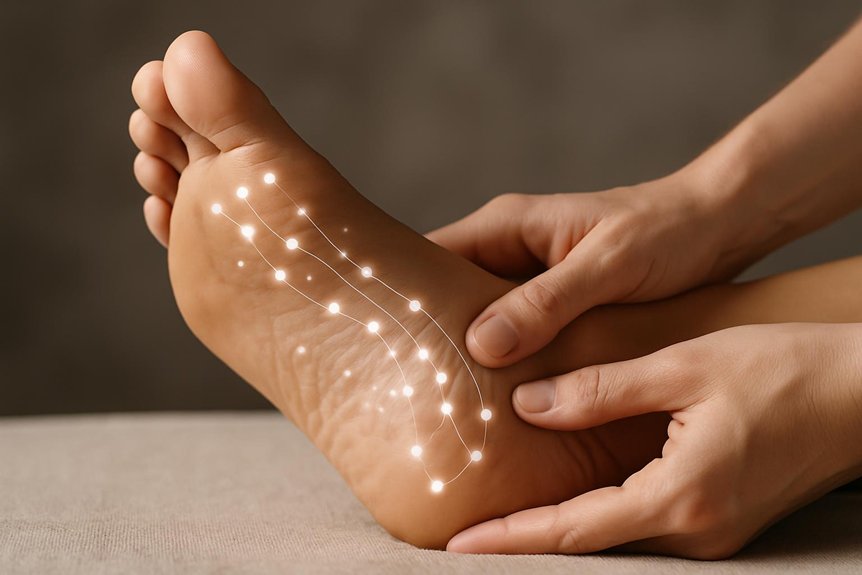
On the reflex therapy foot map, the back is represented primarily along the medial (inner) edge of each foot, where the spinal reflex line is conventionally traced from the hallux (cervical region) down through the arch (thoracic and lumbar regions) to the medial heel (sacrum and coccyx).
Adjacent bands along the inner arch correspond to paraspinal tissues, while the ball of the foot and upper arch relate to shoulder girdle and thoracic tension patterns.
In Spa & Massage clinics, therapists typically apply thumb-walking or slow hook-and-backup pressure along this line, working bilaterally with graded depth to stay within comfortable sensation.
Skin integrity is checked; pressure is reduced over varicosities, neuropathy, acute inflammation, or pregnancy-specific contraindications.
Clients are encouraged to breathe steadily and communicate.
Reflex Therapy Points for Lower Back Pain
For lower back pain, it commonly targets the lumbar–sacral reflex zones along the medial arch and heel margins, assessed bilaterally for tenderness and tissue density.
Clinical application typically uses controlled thumb-walking or sustained pressure at tolerable intensity for 30–90 seconds per point, repeated in short sets with monitoring for adverse sensitivity; Spa & Massage therapists standardise this timing within individualised treatment plans.
Persistent or escalating pain, neurological symptoms (e.g., numbness, weakness), or red flags such as fever or recent trauma warrant prompt medical review, with hands-on care provided only as appropriate support.
Key Foot Zones
Within the reflex point foot map, lower back discomfort is most commonly addressed by targeting the medial longitudinal arch of each foot—particularly the spinal reflex line running from the heel toward the ball—along with the heel’s central-to-inner margin, where lumbar and sacral zones are typically referenced.
Secondary zones include the plantar heel pad (pelvic floor/hip interface) and the inner ankle region, often associated with pelvic girdle support.
At Spa & Massage clinics across London, therapists typically assess both feet for tenderness, asymmetry, temperature change, and tissue density before selecting zones.
Attention is kept close to bony landmarks to avoid compressing sensitive soft tissue unnecessarily.
Skin integrity is checked; areas with acute inflammation, open skin, neuropathy, or suspected fracture are excluded.
Clients are guided to breathe slowly and communicate comfort thresholds.
Pressure Techniques And Timing
Using controlled, incremental pressure, it work for lower back pain typically begins with light-to-moderate “warming” strokes along the spinal reflex line (medial arch) before progressing to sustained thumb-walking and small, precise pivot presses over tender lumbar–sacral zones; pressure is increased only to a tolerable therapeutic threshold (often described as “strong but not sharp”) and reduced immediately if pain, numbness, or radiating sensation occurs.
In Spa & Massage clinics, therapists stabilise the foot with a cradling hold to prevent shearing, then apply 3–6 second compressions with 2–3 second releases to encourage local circulation and neuromuscular down-regulation.
Work is typically sequenced: medial arch, heel margin, then ankle groove, repeating 2–3 passes per foot.
Total focused time is kept to 8–12 minutes, allowing the body to soften without overstimulation.
When To Seek Support
Even with well-calibrated pressure, timing, and careful sequencing over the spinal reflex line and heel margin, lower back symptoms can indicate a presentation that falls outside self-directed reflex therapy.
Support is indicated when pain is acute after a fall, progressive, nocturnal, or paired with fever, unexplained weight loss, saddle numbness, altered bladder or bowel control, or radiating symptoms below the knee with weakness or pins-and-needles.
Pregnancy, anticoagulant use, diabetes-related neuropathy, skin infection, or vascular compromise also warrant clinician-led care.
Spa & Massage therapists advise pausing home work and booking an assessment when tenderness becomes sharp, bruising appears, or the client cannot relax into pressure.
In-clinic reflex therapy can then be adapted—lighter loading, shorter holds, and calming diaphragmatic cueing—while referral is arranged when needed.
Reflex Therapy Points for Mid and Upper Back Pain
Where can zone therapy be applied when discomfort localises in the thoracic (mid-back) or upper back region?
In foot reflex therapy, practitioners map this area to the thoracic spine zone along the medial arch, extending superiorly toward the base of the toes; upper back and shoulder tension may correspond to the upper thoracic strip and the shoulder line beneath the fifth toe.
Complementary hand reflex therapy may target the spinal reflex along the ulnar edge and the upper thoracic area under the little finger.
At Spa & Massage clinics, therapists also assess diaphragm, solar plexus, and lung reflexes to support breathing mechanics that can amplify thoracic strain.
Work is contraindicated over open skin, acute inflammation, suspected fracture, or new neurological symptoms; pregnancy and anticoagulant use warrant clinical screening.
How to Press Reflex Therapy Points for Back Pain Safely
Often, safe self-applied reflex therapy for back pain begins with controlled pressure on the relevant foot or hand zones using the thumb-walk or fingertip “press-and-hold” method (approximately 3–5/10 intensity), maintained for 5–10 seconds per point and repeated 2–3 cycles while monitoring for referred discomfort, numbness, or symptom escalation.
The client should be positioned comfortably, with the ankle or wrist supported, breathing slow and even to prevent guarding.
Pressure is directed perpendicular to tissue, then eased off gradually; sliding friction is avoided to protect skin.
Sensitive areas are approached by “feathering” around the point before settling into a steady hold.
In Spa & Massage clinics, therapists recommend a light, unscented oil to reduce drag and keep touch reassuring, warm, and precise.
Hydration and brief rest follow.
When to Choose Massage or Seek Clinical Help
For mild, non-specific back pain without red-flag symptoms, clients may choose manual therapy—such as deep tissue or sports massage at Spa & Massage—to reduce myofascial tension, improve local circulation, and support functional movement alongside zone therapy.
Escalation to clinical assessment is indicated when pain is severe, progressive, post-traumatic, or accompanied by neurological signs (numbness, weakness, radiating leg pain), bowel/bladder changes, fever, unexplained weight loss, or night pain. In such cases, massage should be deferred until a medical professional has ruled out serious pathology and provided appropriate management guidance.
Massage For Mild Back Pain
In cases of mild, non-specific back discomfort, massage may be an appropriate first-line option when symptoms are muscular in origin (e.g., postural tension, overuse, or localised myofascial tightness) and there are no red-flag indicators.
At Spa & Massage clinics, therapists typically select deep tissue or sports techniques with graded pressure, focusing on paraspinals, quadratus lumborum, gluteals, and hip flexors to reduce tone and improve segmental mobility. Slow effleurage and sustained trigger-point compression may be combined with gentle myofascial release to soften adhesions and support calmer breathing.
Treatment is kept within comfortable limits, with ongoing consent and feedback. Aftercare usually includes hydration, heat, and brief mobility drills; many clients also choose reflex therapy as a soothing adjunct for whole-body downregulation.
Signs You Need Medical Help
Alongside hands-on therapies, safe back-pain management begins with triage: massage is appropriate for non-specific, muscular pain that is stable or improving, whereas new or escalating symptoms, neurological signs, or systemic features require clinical assessment before any bodywork.
Spa & Massage advises medical review for red flags: leg weakness, foot drop, saddle numbness, new bladder or bowel dysfunction, progressive sciatica, unexplained fever, night sweats, unintentional weight loss, history of cancer, significant trauma, osteoporosis, or anticoagulant use.
Urgent care is also indicated when pain is constant at rest, wakes the client nightly, or follows infection or recent surgery.
When cleared, therapists use light pressure, neutral spinal positioning, and consent-led draping; deep tissue, vigorous stretches, and reflex therapy points are deferred until stability and diagnosis are confirmed.
Conclusion
It is for back pain targets mapped zones along the medial foot arch and heel, aiming to down‑regulate sympathetic tone and reduce myofascial guarding. Like an old cartographer tracing the spine in miniature, the practitioner applies graded, tolerable pressure, monitoring tissue reactivity and client feedback. Benefits are typically adjunctive, supporting relaxation, sleep quality, and perceived pain modulation. Aftercare emphasises hydration, gentle mobility, and avoiding provocative loading. Persistent, progressive, or neurological symptoms warrant prompt clinical assessment.