It can help psoas-related tightness when symptoms are driven by myofascial restriction and protective guarding in the iliopsoas complex and adjacent tissues such as iliacus, TFL, adductors, quadratus lumborum, and abdominal fascia. Treatment uses slow, graded pressure and breath-led downregulation to reduce tone and improve hip extension without aggressive, invasive abdominal compression. A clinician should screen for referred pain patterns and red flags like fever, night pain, or neurological changes. Further details clarify who benefits most and typical session planning.
Can It Help Psoas Tightness?

How effectively can itreduce psoas tightness? It can help when tightness is driven by myofascial restriction in the iliopsoas complex and adjacent tissues, including the iliacus, quadratus lumborum, diaphragm, and anterior hip capsule.
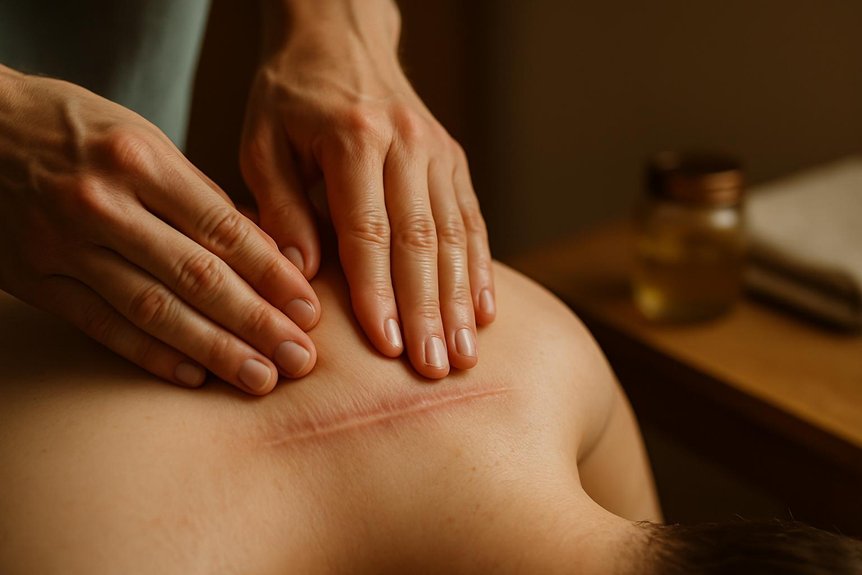
At Spa & Massage clinics across London, therapists assess pelvic position, lumbar tone, and hip rotation, then apply slow, graded pressure to hip flexors, adductors, and abdominal fascia, avoiding unsafe compression of visceral structures.
Deep tissue work uses slow, sustained techniques to target deeper muscle and fascia layers, supporting improved mobility and reduced discomfort through deep tissue massage methods.
Treatment is paired with breath-led downregulation and gentle, close-contact positioning so the client feels held while tissues soften.
Many clients benefit from reduced guarding and improved hip extension after several sessions, supported by home mobility and hydration guidance.
What Does Psoas Tightness Feel Like?
Psoas tightness commonly presents as a deep ache or sharp pulling sensation in the front of the hip, groin, or lower back, sometimes referring into the abdomen or thigh.
Clients may notice restricted hip extension, discomfort when standing upright after sitting, and reduced stride length, with compensations that increase lumbar lordosis or anterior pelvic tilt.
In Spa & Massage clinics, therapists assess these symptom patterns alongside posture and movement to guide a client-centred treatment plan.
Common Sensations And Pain
Often, tightness in the iliopsoas complex presents as a deep, hard-to-localise ache at the front of the hip or groin, with symptoms commonly referring into the lower back, pelvis, or upper thigh and intensifying during hip extension (e.g., walking stride), prolonged sitting, rising from a chair, or sustained standing.
Some clients describe a gripping or “caught” feeling deep behind the abdominal wall, with tenderness near the inner hip crease and a guarded, protective response to touch. Discomfort may radiate towards the sacroiliac region, pubic area, or anterior thigh, sometimes alongside a dull lumbar heaviness.
In more irritable cases, there can be sharp stabs with pivoting, coughing, or sneezing due to increased intra-abdominal pressure. At Spa & Massage, therapists assess referral patterns and irritability to tailor pressure and pacing safely.
Movement Limits And Posture
In day-to-day movement, iliopsoas tightness typically shows up as reduced hip extension and altered lumbopelvic control, prompting compensations such as increased lumbar lordosis, anterior pelvic tilt, or an abbreviated stride.
Clients often notice difficulty fully standing tall after sitting, a pulling sensation at the front of the hip, or low-back “gripping” during walking, running, or climbing stairs.
Prolonged sitting can amplify this pattern, making the pelvis feel drawn forward and the abdomen feel tense.
In supine lying, some feel unable to let the low back rest heavy, as if the hip flexors are keeping guard.
At Spa & Massage, therapists observe that these postural habits may limit glute recruitment and deepen discomfort; treatment is paired with gentle hip-extension drills.
Is It Really Your Psoas (and Red Flags)?
Where is the discomfort felt—and does it actually follow the psoas’ anatomy? True psoas-related pain is often deep in the lower abdomen or front of the hip, sometimes referring to the groin, and may feel sharper when lifting the knee or extending the hip.
Lateral hip pain, buttock ache, or pain centred over the low back joints more often implicates gluteals, hip flexor tendons, lumbar facets, or the sacroiliac region rather than the psoas itself.
Spa & Massage therapists screen carefully and refer out when red flags appear: fever, unexplained weight loss, night pain, bowel or bladder changes, numbness or weakness, recent trauma, pregnancy complications, or escalating pain unrelieved by rest.
Why London Life Tightens Your Psoas

In London, prolonged desk hours and habitual sitting keep the hips in flexion, encouraging the psoas to remain shortened and over-recruited. Commuting—especially Tube posture with forward head carriage and a tucked pelvis—can further load the hip flexors and reduce efficient glute engagement during standing and walking.
Chronic stress can also elevate tone through shallow, upper-chest breathing patterns that limit diaphragmatic excursion, and Spa & Massage therapists often observe this breathing–tension link when evaluating clients with anterior hip tightness.
Desk Hours And Sitting
Often, long desk hours and regular commuting across London place the hips in sustained flexion, keeping the psoas shortened and under continuous low-level load. Over time, this hip-flexor dominance can inhibit glute activation, alter pelvic tilt, and increase lumbar compression, felt as deep groin tightness or an ache at the front of the hip.
Clients may notice reduced hip extension during walking, shallow breathing, or a guarded abdomen, as the psoas blends with the diaphragm and fascial chains. At Spa & Massage clinics, therapists assess sitting-related patterns and may use deep tissue and myofascial techniques around the iliacus, rectus femoris, and adductors to ease protective tone, while guiding gentle movement breaks and hip-opening stretches for safer daily relief.
Commuting And Tube Posture
On the Tube, habitual standing with the pelvis tucked, ribs flared, and one hip “hung” into a handrail—or prolonged sitting on a narrow seat with knees higher than hips—keeps the psoas and iliacus in sustained shortening while the lumbar spine stabilisers fatigue.
Over time, this bias pulls the lumbar vertebrae forward and narrows hip extension, often felt as a deep front‑hip grip, low-back ache, or a “stuck” stride after walking.
Clients who commute daily may also develop asymmetry from always loading one leg or rotating to check doors and phones.
At Spa & Massage, therapists assess pelvic tilt, hip rotation, and tenderness along the iliopsoas line, then use deep tissue and myofascial techniques to ease tone and restore comfortable, grounded standing in the body.
Stress, Breathing, And Tension
Under chronic stress, the nervous system shifts toward sympathetic dominance, subtly recruiting the hip flexors as part of a whole‑body “bracing” strategy.
In London, deadlines, noise, and crowded travel can maintain low‑grade guarding through the iliopsoas, compressing the anterior hip and limiting extension.
Shallow, upper‑chest breathing increases accessory respiratory muscle tone and often couples with an anterior pelvic tilt, further shortening psoas fibres and sensitising nearby lumbar segments.
Clients may notice a constant “held” feeling deep in the abdomen or groin, plus aching in the low back.
At Spa & Massage clinics across London, therapists assess breath, rib mobility, and pelvic position, then apply deep tissue and myofascial techniques with slow pacing to invite parasympathetic settling and safer hip lengthening.
Can Deep Tissue Reach the Psoas Safely?
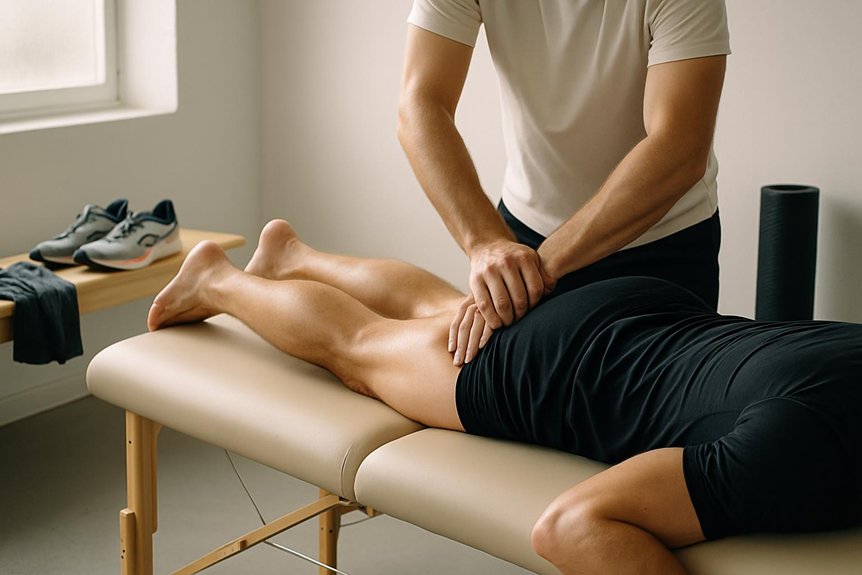
A tight psoas sits deep in the abdomen and pelvis, behind the abdominal wall and close to sensitive structures, so it cannot be “dug into” like a superficial hip flexor. Safe access relies on indirect, graded pressure through the lower abdomen and iliacus region, guided by breath, guarding, and tissue tone rather than force.
At Spa & Massage, therapists keep contact slow and consensual, working within a client’s comfort to avoid compressing bowel, bladder, or vessels. Hip positioning (slight flexion and external rotation) can soften the abdominal wall, allowing gentle sinking toward the muscle belly.
Clear communication, draping, and permission before any lower-abdominal work protect boundaries while maintaining intimacy. Sharp pain, nausea, or pulsing sensations are treated as stop signals.
Deep Tissue vs Sports Massage for Psoas

Most clients with psoas-related tightness benefit from either intensive tissue massage or sports massage, but the clinical rationale differs.
Deep tissue work is selected when the goal is to reduce guarded tone in the hip flexor complex and adjacent fascia—iliacus, rectus femoris, TFL, and abdominal wall—so the psoas can soften indirectly without invasive pressure.
Sports massage is chosen when symptoms relate to training load, hip flexion bias, or running mechanics, using more specific, performance-led sequencing around gluteals, adductors, and lumbar stabilisers.
At Spa & Massage clinics across London, therapists assess breathing, pelvic tilt, and tenderness, then choose pressure, pacing, and draping that feels safe and close.
Deep tissue often suits chronic, stress-linked holding; sports massage suits activity-linked flare-ups.
Stretches After Deep Tissue for Psoas
Following deep tissue work for psoas-related tightness, carefully dosed stretching helps consolidate reduced hip-flexor tone while maintaining a neutral pelvic position and unforced lumbar alignment.
At Spa & Massage clinics, therapists suggest low-load holds: half-kneeling hip-flexor stretch with a gentle posterior pelvic tilt and soft glute engagement; supine “Thomas” position off a bed edge to lengthen iliopsoas without rib flare; and supported child’s pose with slow lateral breathing into the lower abdomen to reduce guarding.
Each stretch is held 20–40 seconds, 2–3 rounds, staying below sharp sensation.
The client is encouraged to feel warmth and spaciousness in the groin and deep front hip, while keeping the neck, jaw, and pelvic floor relaxed and easy.
How Many Sessions for Psoas Tightness?
Estimating session frequency for psoas-related tightness depends on tissue irritability, chronicity, and the drivers sustaining hip-flexor tone (prolonged sitting, anterior pelvic tilt, lumbar overextension, or load from running and lifting).
For recent, mild guarding, Spa & Massage therapists often suggest 1–2 deep tissue or sports massage sessions weekly for 2–3 weeks, then reassess tone, hip extension, and lumbar comfort.
For longstanding tightness with pelvic asymmetry or low-back referral, a 4–6 session plan may be needed, spaced 5–10 days apart, integrating gluteal and abdominal wall work to reduce psoas load.
Many clients maintain results with monthly sessions plus tailored mobility and breath-led pelvic floor relaxation, supporting a softer, safer sense of openness through the front of the hip.
Conclusion
It may reduce perceived psoas “tightness” by decreasing tone in adjacent hip flexors, abdominals, lumbar fascia, and gluteal stabilisers, while improving pelvic mechanics. Direct psoas contact is not always necessary and should be performed only when clinically indicated and safely tolerated. For example, a desk-based runner with anterior hip pain and lumbar stiffness improved after four sessions focused on iliacus, rectus femoris, and quadratus lumborum, followed by graded hip-extension drills.