It can help reduce runner’s knee (patellofemoral pain) symptoms short term by decreasing muscle guarding and pain sensitivity around the hip, thigh, and lower leg. It is best used as an adjunct to a structured rehabilitation plan that addresses load spikes, hip abductor/external rotator strength, and quadriceps capacity. Sessions often target vastus lateralis, TFL, gluteals, and calf trigger points while avoiding aggressive pressure over irritated tissues. Further guidance covers scheduling, aftercare, and red flags.
What Is Runner’s Knee, and Why Does It Flare Up?

Runner’s knee—most commonly patellofemoral pain syndrome—is an overuse-related anterior knee pain pattern centred around irritation of the tissues surrounding the kneecap (patella) and its tracking over the femur.
Symptoms often include diffuse ache behind or around the patella, worse with stairs, hills, squats, or prolonged sitting, and sometimes crepitus without swelling.
Flares are typically driven by load spikes: sudden mileage increases, speedwork, downhill running, or reduced recovery.
Contributing factors include hip abductor/external rotator weakness, quadriceps capacity deficits, calf/ankle stiffness, and reduced control of femoral internal rotation, which can increase patellofemoral joint stress.
Footwear changes, hard surfaces, and training fatigue may amplify sensitivity.
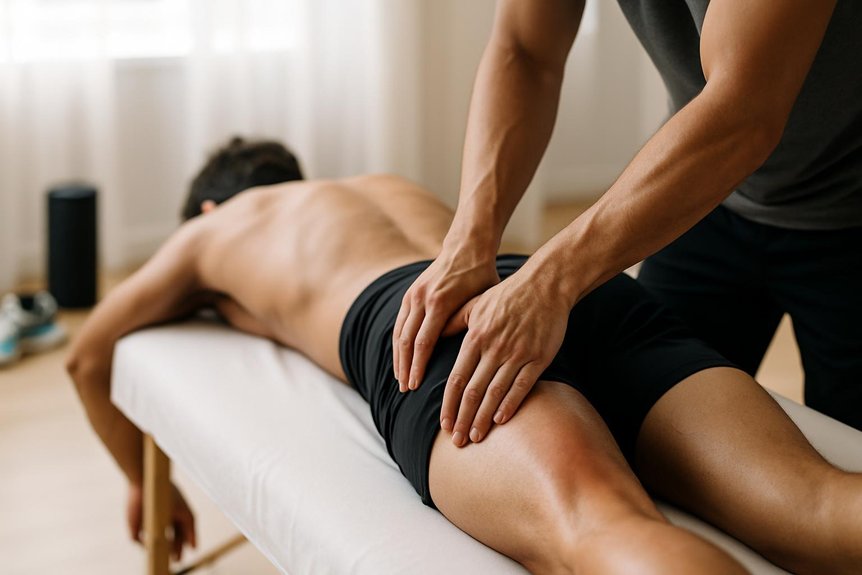
Deep tissue massage techniques can help by addressing muscle tension and improving soft-tissue mobility in overloaded areas.
At Spa & Massage, therapists commonly screen movement and tenderness patterns to guide supportive, individualised care.
Does Intensive Tissue Massage for Runner’s Knee Help Pain?
It may help reduce runner’s knee pain by decreasing myofascial tension around the hip, thigh, and lower leg, improving local circulation, and modulating pain sensitivity.
In Spa & Massage clinics, therapists commonly target trigger points in structures such as the quadriceps, iliotibial band region, and gluteal muscles to offload stress at the patellofemoral joint. Relief can be immediate but often builds over several sessions, with treatment frequency typically guided by symptom irritability, training load, and response over 24–48 hours.
How Massage Eases Pain
For many cases of anterior knee pain associated with running, massage can help reduce symptoms by addressing soft‑tissue contributors rather than the joint surface itself. Manual pressure and slow strokes can decrease protective muscle guarding around the quadriceps, hip rotators, and lateral thigh, easing tensile load transmitted toward the patellofemoral joint.
Massage may also improve local circulation and fluid exchange, supporting recovery in irritated tendons and fascia, and it can down‑regulate pain through calming sensory input to the nervous system. In Spa & Massage clinics across London, therapists assess movement and tenderness, then apply deep tissue or sports techniques within a comfortable, communicative pressure range, helping clients feel safely held while tissues soften. Short-term symptom relief can make strengthening and gait retraining more tolerable between runs.
Targeting Trigger Points
Pain reduction from manual therapy is often linked to changes in muscle tone and sensitivity, and one specific focus is myofascial trigger points—localised hyperirritable nodules within taut bands that can refer pain toward the front of the knee.
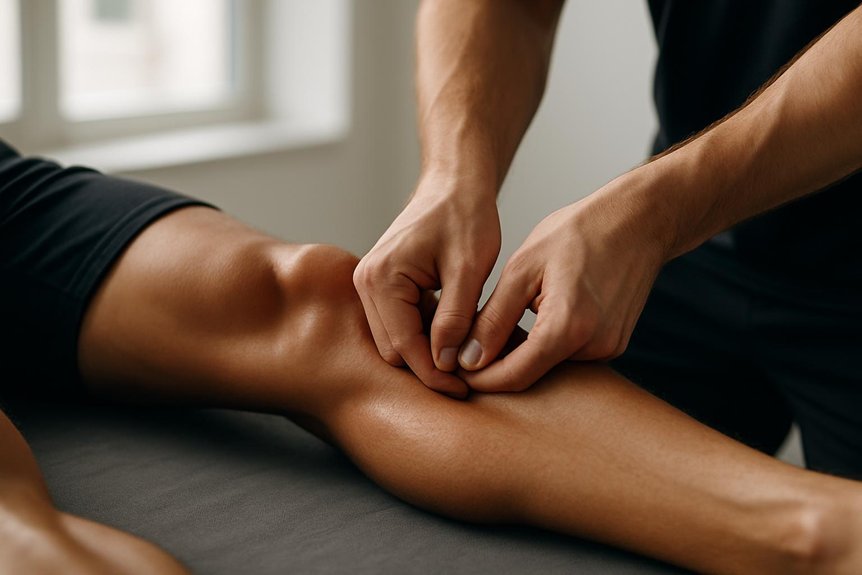
In runner’s knee, common sources include the vastus lateralis, rectus femoris, tensor fasciae latae, gluteus medius, and lateral gastrocnemius, which may increase patellar tracking stress and amplify soreness with stairs or running.
At Spa & Massage clinics, therapists use slow, specific deep-tissue pressure, friction, and short sustained holds to “deactivate” these points, then recheck tenderness and knee comfort during simple movements.
Pressure is kept within a tolerable, safe intensity, encouraging release without provoking protective guarding.
Many clients notice less sharp, spreading pain and easier knee bending immediately after treatment.
Relief Timeline And Frequency
Often, symptom change from manual therapy for runner’s knee follows a staged timeline rather than an immediate “fix”: some individuals report a same‑day drop in diffuse ache and improved knee bend after a session, while more durable gains typically require repeated treatments over 2–6 weeks alongside load modification and strengthening.
In Spa & Massage clinics, therapists commonly schedule 1 session weekly for 2–3 weeks, then taper to every 10–14 days as irritability settles.
High‑sensitivity knees may respond better to shorter, lower‑pressure work initially, with deeper techniques added once post‑session soreness is minimal.
A useful benchmark is reduced pain during stairs or a short run within 48–72 hours.
If pain spikes, persists beyond two days, or swelling increases, frequency should be reduced and training volume reviewed.
Which Muscles Does Intensive Tissue Massage Target for Runner’s Knee?
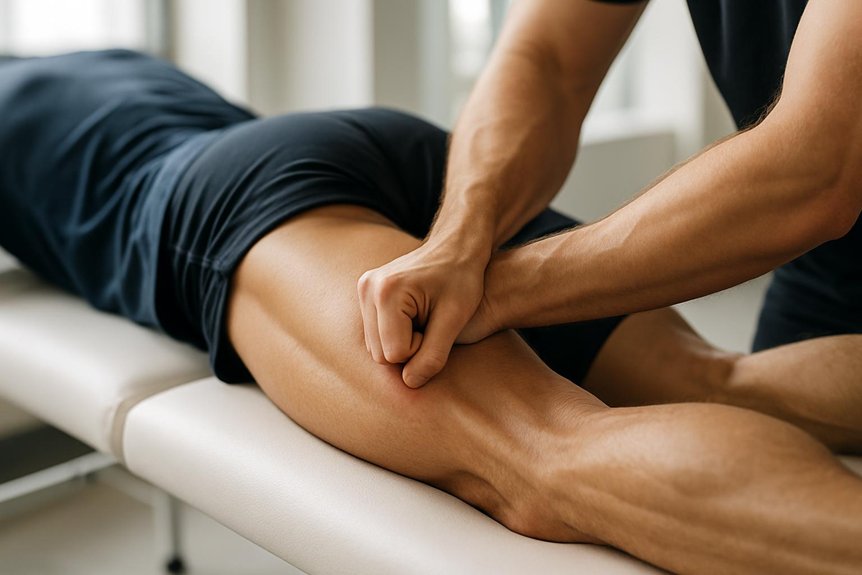
Runner’s-knee symptoms commonly reflect overload and altered tracking at the patellofemoral joint, so intensive tissue massage is typically directed beyond the front of the knee to the tissues that drive femoral and tibial mechanics.
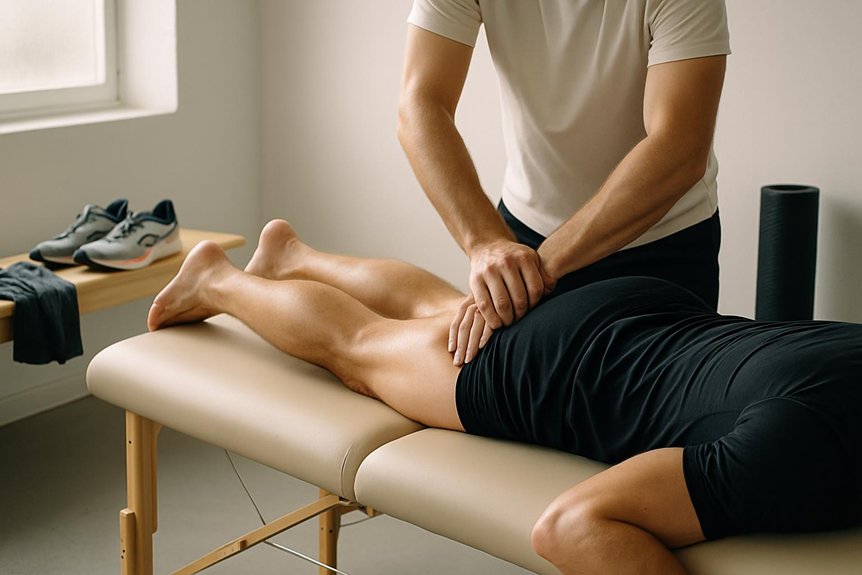
At Spa & Massage, therapists commonly target the lateral thigh—tensor fasciae latae and the iliotibial band interface—plus vastus lateralis and rectus femoris, when tone biases the patella outward.
The hip abductors and external rotators (gluteus medius, gluteus maximus, deep rotators) are addressed when femoral internal rotation contributes to pain.
Posterior-chain structures—hamstrings and gastrocnemius/soleus—may be treated to reduce traction and improve knee extension mechanics.
Adductors and the hip flexors are included if pelvic control and stride length are limited.
What Happens in a Runner’s Knee Deep Tissue Session?
In a runner’s knee deep tissue session at Spa & Massage, the therapist begins with a brief clinical assessment of pain location, training load, and movement patterns to identify the primary soft-tissue contributors to anterior knee symptoms.
Treatment then targets relevant myofascial restrictions using graded deep tissue and sports-massage techniques, with pressure adjusted to tissue response and symptom behaviour.
Aftercare guidance is provided to support recovery, typically including load modification, hydration, and simple self-management strategies aligned with the findings.
Assessment And Treatment Focus
Before any hands-on work begins, a runner’s knee deep tissue session at Spa & Massage is structured around a brief clinical-style assessment—clarifying pain location and training load, checking aggravating movements (such as stairs, squats, or prolonged sitting), and screening hip, knee, and ankle mobility—to identify the most likely contributing tissue restrictions and load-management issues that will guide the treatment focus.
Palpation then maps tenderness and tone across the lateral thigh, quadriceps, adductors, gluteals, and calf, while comparing sides for asymmetry.
Particular attention is given to the iliotibial band region, patellar tendon, and retinaculum, noting irritability and swelling risk.
Treatment focus is framed as reducing excessive lateral pull, easing compressive load at the patellofemoral joint, and supporting more comfortable tracking.
Consent, pressure preferences, and emotional comfort are checked throughout.
Techniques And Aftercare Guidance
Following the assessment, a runner’s knee deep tissue session at Spa & Massage typically uses targeted, tolerance-led techniques—such as slow myofascial release to the lateral thigh and hip, deep longitudinal strokes through quadriceps and adductors, trigger point work in gluteals and calf, and careful soft-tissue mobilisation around the patellar tendon and retinaculum—to reduce local tone and sensitivity without provoking post-treatment flare.
Pressure is progressed only with clear consent, staying in a “strong but safe” range to support comfort and trust.
Many sessions finish with soothing effleurage and brief coaching on pain-calming breath to downshift guarding.
Aftercare usually includes hydration, gentle walking, and 24–48 hours of reduced hill or speed work.
In-clinic guidance may add light stretching, heat if stiff, or ice if irritable, plus symptom tracking.
How Should You Combine Massage With Runner’s Knee Rehab?
Alongside a structured rehabilitation programme, massage should be integrated as an adjunct to reduce pain, improve local tissue mobility, and support adherence to progressive loading in runner’s knee. At Spa & Massage, therapists time sessions around exercise: ideally 24–48 hours after heavier strength work, or the evening before technique drills, to help the knee feel calmer without masking symptoms.
Massage targets lateral thigh, quadriceps, hip rotators, and calf to reduce excessive tension that can alter patellar tracking; direct deep pressure over an irritated patellar tendon or acutely painful retinaculum is avoided.
Rehab remains primary: hip abductor and quad strengthening, gradual return-to-run, and mobility work. Clients are advised to treat post-massage soreness like training DOMS, then resume the plan at the next scheduled dose consistently.
When Should You Stop and See a Clinician Instead?
Massage can support runner’s knee rehabilitation, but it should not be used to manage symptoms that suggest a more serious injury or a condition requiring medical assessment.
A clinician should assess locking, true giving way, rapid swelling within hours, deformity, inability to weight-bear, or pain after a fall or twist.
Urgent review is also indicated with fever, redness, heat, calf swelling, numbness, or night pain.
If symptoms persist beyond 2–3 weeks despite reduced load, or worsen with basic walking, assessment helps rule out meniscal injury, patellofemoral instability, stress fracture, or referred hip pathology.
At Spa & Massage, therapists screen these red flags, pause treatment, and recommend GP, physiotherapy, or imaging.
Massage then resumes as a supportive, comfortable adjunct.
Conclusion
Intensive tissue massage may reduce runner’s knee symptoms by improving tolerance to load and easing soft‑tissue sensitivity in the quadriceps, calves, and hip rotators, but it is not a stand‑alone fix. Best outcomes occur when massage supports progressive strengthening, gait or training adjustments, and activity pacing. For example, a 34‑year‑old London runner with pain on stairs used weekly deep tissue sessions plus hip and quadriceps rehab; within four weeks, pain fell and mileage resumed gradually.