It can help shin splints (medial tibial stress syndrome) by reducing calf and lower‑leg soft‑tissue tension, trigger points, and fascial restriction that contribute to tibial loading pain. Techniques such as slow deep strokes, myofascial release, and targeted compression may improve tissue glide, ease post‑exercise tightness, and support a graded return to running when paired with load modification. However, overly aggressive or poorly timed treatment can worsen symptoms, and focal or night pain warrants assessment. Further details clarify candidates, targets, and safe session planning.
Can It Help Shin Splints Pain?

In many cases, sports massage can help reduce shin splints pain by addressing the soft‑tissue contributors to medial tibial stress syndrome, particularly excessive tension and trigger points in the calf complex and surrounding fascia.
By improving tissue glide and reducing local sensitivity, it may decrease pain during daily loading and short runs, and support gradual return to training when paired with activity modification.
Because it’s often used as part of the benefits of athletic massage for athletes, it may also support recovery by improving circulation and easing post‑exercise muscle tightness.
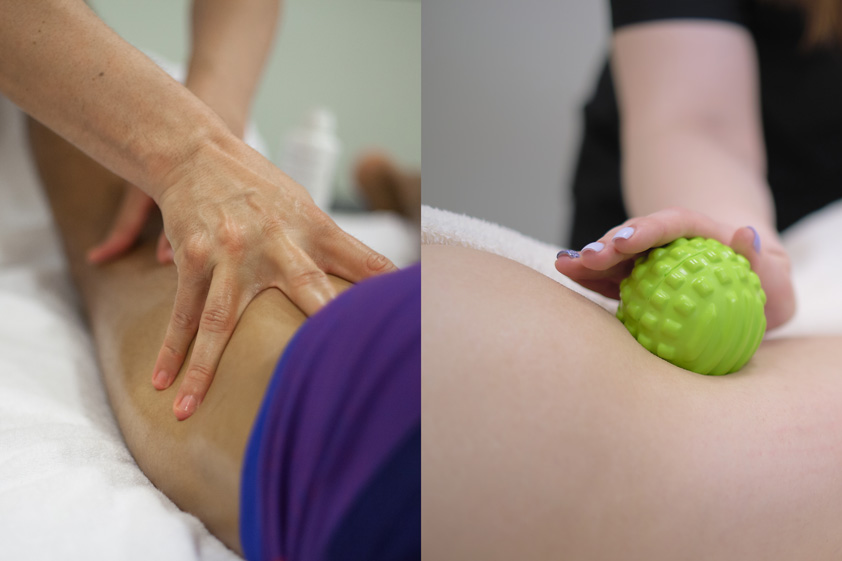
At Spa & Massage clinics in London, therapists typically use slow, deep strokes, myofascial release, and targeted trigger‑point work to the gastrocnemius, soleus, and tibialis posterior, staying within tolerable discomfort.
Many clients prefer discreet draping and clear consent, allowing close, focused work while maintaining comfort.
Aftercare commonly includes gentle calf mobility, hydration, and 24–48 hours of reduced impact.
What Causes Shin Splints in Runners?
Shin splints in runners are most commonly associated with training load errors and repetitive overuse that exceed the tibial and soft-tissue capacity to adapt.
Contributing factors often include biomechanical patterns such as excessive pronation, reduced ankle mobility, or altered hip control, which can increase traction and bending stress along the tibia.
Footwear that provides inadequate support and running on harder or cambered surfaces may further amplify impact forces and cumulative tissue strain.
Training Load And Overuse
Increase training volume too quickly and the lower leg often fails to adapt, making excessive training load and repetitive impact the primary drivers of medial tibial stress syndrome (commonly termed “shin splints”) in runners.
Common triggers include abrupt mileage increases, adding speed sessions, or returning after time off without progressive conditioning, leading to cumulative microtrauma along the tibial border.
Early symptoms—tenderness and aching during or after runs—often reflect overload exceeding tissue recovery capacity; continuing to “run through it” can prolong inflammation and elevate stress-injury risk.
At Spa & Massage, therapists often note coexisting calf tightness and fatigue that amplify strain during repeated foot strikes.
Practical load control includes reducing intensity, spacing high-impact sessions, and using short-term cross-training while symptoms settle.
Gradual progression protects.
Biomechanics, Footwear, Surfaces
Beyond simple training load, medial tibial stress syndrome is strongly influenced by lower-limb biomechanics and the external conditions underfoot. Excessive pronation, reduced ankle dorsiflexion, and hip control deficits can increase tibial bending and traction on the periosteum, sensitising the inner shin. Footwear that is overly worn, unsupportive, or mismatched to foot type may fail to manage impact and rotation, especially during higher-mileage blocks.
Surface changes also matter: repeated running on cambered roads, uneven pavements, or very hard ground concentrates stress through the tibia and posterior calf complex. At Spa & Massage clinics, therapists often screen calf and tibialis posterior tension and advise gradual shifts in shoes and surfaces, helping runners feel held, informed, and safer while returning to consistent training.
What Does It Target for Shin Splints?
For shin splints, it typically targets excessive lower-leg muscle tension—particularly in the calf complex and tibialis muscles—where increased tone can elevate traction forces along the medial tibial border.
It also addresses fascial restriction and cumulative tendon load to help reduce local mechanical stress and support more efficient force transfer during running.
At Spa & Massage, therapists assess these tissue contributors and apply targeted athletic massage techniques to modulate load-sensitive structures while staying within symptom tolerance.
Lower-Leg Muscle Tension
Most cases of shin splints (medial tibial stress syndrome) involve excessive tension and overload in the lower-leg musculature—particularly the calf complex (gastrocnemius and soleus), tibialis posterior, tibialis anterior, and the connective tissues that transmit their pull onto the tibial border—so it is typically directed at reducing myofascial tightness, improving tissue glide, and lowering abnormal traction forces that aggravate pain along the shin.
At Spa & Massage clinics, therapists assess tone, tenderness, and trigger points, then apply slow deep-tissue strokes, compression, and gentle stripping along the calf and anterior shin to calm guarding and restore comfortable range.
Pressure is kept within a “good pain” window, encouraging relaxation without flaring symptoms. Many clients are advised on hydration, heat, and light mobility between sessions to maintain softness and reduce recurrent overload.
Fascial And Tendon Load
Offload the shin by addressing the connective-tissue system that transmits force into the tibial border.
In medial tibial stress syndrome, excessive fascial tension and tendon traction (notably along the soleus–deep posterior compartment and tibialis posterior pathway) can concentrate load where the periosteum is sensitive.
It targets these interfaces to reduce stiffness, improve glide, and modulate pain, supporting better load distribution during running and walking.
At Spa & Massage clinics, therapists may use slow, specific myofascial techniques and cross-fibre work around the calf–Achilles–medial ankle line, staying within a tolerable “good pressure” that feels safe and personal.
This is paired with calf and foot mobility advice and graded return-to-load to protect healing.
When Can It Worsen Shin Splints?
In certain cases, it can exacerbate shin splints by increasing mechanical load and inflammatory irritation in already sensitised tissues along the tibial border.
Risk rises when pressure is deep, fast, or directly on the painful periosteal area, provoking protective guarding and post-treatment flare. It may also worsen symptoms during the acute, reactive phase, when tenderness, heat, or swelling signal heightened nociception.
Aggressive stripping of tibialis posterior or soleus can increase traction on the medial tibia, amplifying symptoms during running.
Poor timing—immediately before high-impact training—or inadequate clinical screening for stress fracture red flags (night pain, focal bony point tenderness) elevates harm.
At Spa & Massage, therapists avoid “no pain, no gain,” prioritising graded, tissue-respectful work and clear feedback throughout.
What Should You Do at Home for Shin Splints?
At home, shin splints are best managed with short-term load modification and simple symptom-guided measures that reduce tibial stress while maintaining lower-limb capacity. Symptoms typically settle with 3–7 days of reduced running volume, avoiding hills and speedwork, and cross-training that stays pain-free. Ice can be used 10–15 minutes after activity for comfort.
Gentle calf and soleus stretching, plus daily foot-ankle strengthening (heel raises, tibialis anterior raises) helps restore load tolerance. Supportive footwear and temporary arch support may reduce provocation; worn shoes should be replaced.
Self-massage of the calf (not directly on the tender tibial border) can ease tone; in Spa & Massage clinics, therapists emphasise comfortable pressure and hydration after. Seek assessment if pain is focal, worsening, or present at rest/night.
How Many Athletic Massage Sessions Help Shin Splints?
Expect a short course of athletic massage—rather than a single appointment—to provide the most meaningful support for shin splints. Most clients improve with 3–6 sessions over 2–4 weeks, adjusted to pain severity, training load, and tissue irritability.
In early stages, weekly treatment helps calm calf and tibial fascia tension, reduce protective guarding, and restore comfortable ankle motion. As symptoms settle, sessions may space to every 10–14 days to reinforce load tolerance and prevent recurrence.
At Spa & Massage clinics across London, therapists reassess tenderness, morning pain, and hopping tolerance each visit, then tailor pressure and pacing to keep the work therapeutic, never overwhelming. If pain persists beyond 6 sessions, a medical review and graded rehab plan are advised.
Conclusion
It may support shin splints management by reducing calf and tibialis muscle tension, improving soft‑tissue mobility, and aiding short‑term symptom relief alongside load modification. However, it is not a standalone treatment, and aggressive techniques can aggravate irritable periosteal tissues in early or severe cases. Who benefits most—someone continuing impact training, or someone pairing massage with graded return, strengthening, footwear review, and home care? Persistent, focal, or worsening pain warrants clinical assessment.