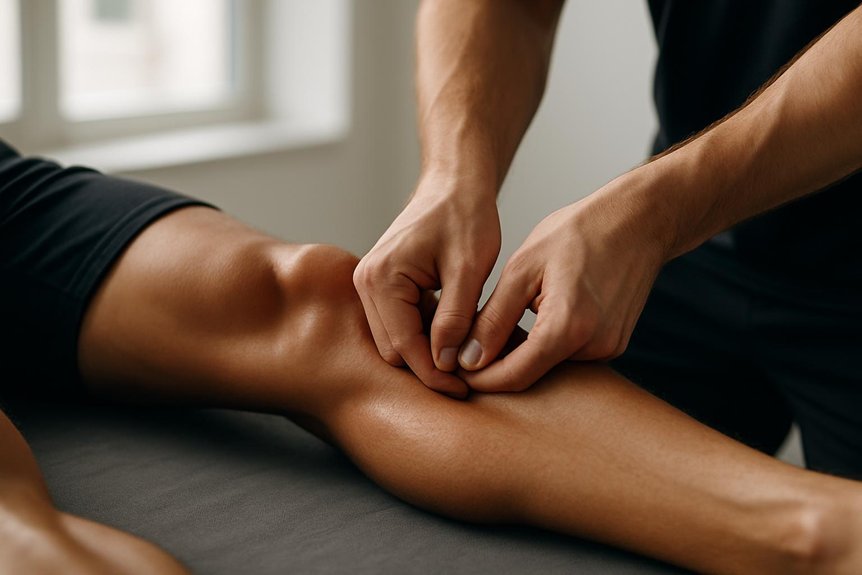
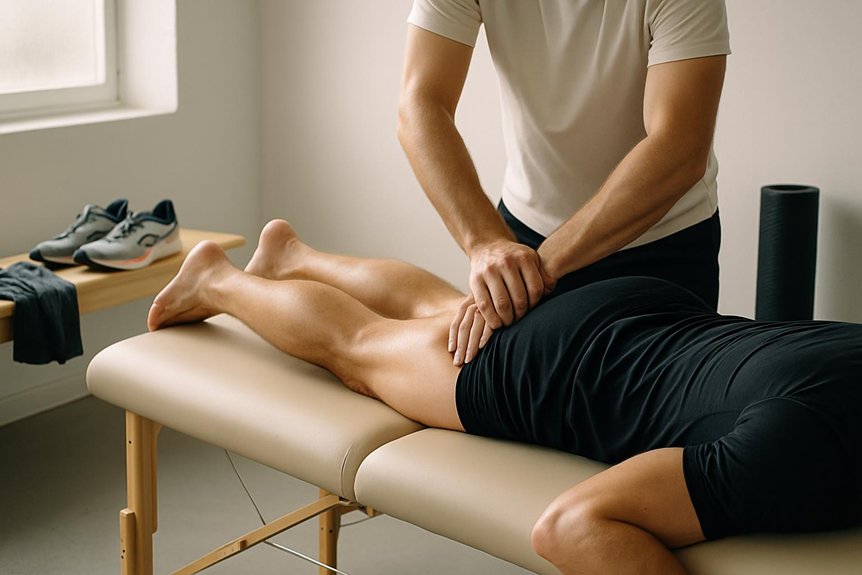
It may help shin splints (medial tibial stress syndrome) by reducing excessive tone and myofascial restriction in the calf and tibialis posterior/anterior, which can increase traction along the medial tibial border. Slow, sustained pressure and trigger-point work can improve local circulation, ease tenderness, and support ankle mechanics, but it works best alongside load management and a gradual return to running. Severe swelling, focal bone pain, night pain, or DVT-type signs need urgent assessment, with practical guidance outlined next.
Can It Help Shin Splints?
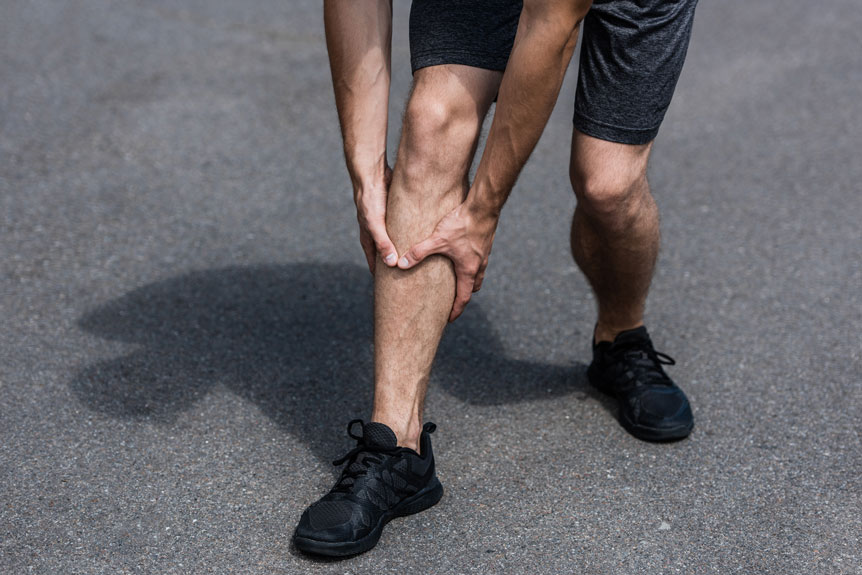
In many cases, deep tissue massage can help manage shin splints (medial tibial stress syndrome) by reducing excessive muscle tone and myofascial restriction in the calf complex—particularly the soleus, gastrocnemius, and tibialis posterior—which can contribute to traction stress along the medial tibial border.
At Spa & Massage clinics, therapists typically combine slow, sustained pressure with targeted trigger-point work to improve local circulation, reduce tenderness, and support comfortable ankle mechanics during walking and running.
It is not a standalone cure, but it can be a valuable adjunct alongside load management and gradual return to activity. It uses slow sustained pressure to address deeper layers of muscle and connective tissue.
Sessions are kept within “good pain” levels, with clear consent and soothing, supportive pacing.
Aftercare often includes gentle calf stretching, hydration, and a short period of rest to let tissues settle.
Do I Have Shin Splints? Signs and Causes
Shin splints (medial tibial stress syndrome) typically present as diffuse tenderness or aching along the inner border of the tibia that worsens with running, jumping, or brisk walking and may ease with rest early on.
Symptoms are commonly triggered by sudden training-load increases, harder surfaces, or inadequate recovery, with pain often recurring at the start of activity and building as exercise continues.
Likely underlying causes include repetitive tibial loading with traction from the calf muscles, biomechanical factors such as overpronation, and strength or flexibility deficits—patterns Spa & Massage therapists routinely assess when advising on massage and self-care.
Common Shin Splint Symptoms
Often, medial tibial stress syndrome (“shin splints”) presents as a diffuse, aching pain along the inner border of the tibia that develops during or after running, jumping, or brisk walking, with local tenderness to touch and symptoms that may ease as the body warms up but return with continued loading.
Pain is typically spread over several centimetres rather than a single pinpoint spot, and pressing the shin can feel bruised or raw.
Mild swelling or tightness in the calf, along with soreness in the tibialis posterior or soleus, may accompany it.
Discomfort can linger for hours after activity and feel worse first thing in the morning.
At Spa & Massage clinics, therapists note clients often report altered gait, reduced ankle mobility, and sensitivity when stretching the calf.
Persistent night pain suggests alternative diagnoses.
Typical Pain Triggers
Medial tibial stress syndrome typically becomes more recognisable when the pattern of symptoms is linked to specific load-related triggers.
Pain often appears during or shortly after running, brisk walking, jumping, or hill work, then settles with rest, only to return when training resumes. Symptoms commonly flare with sudden increases in distance, pace, frequency, or harder surfaces, and may be provoked by longer periods on the feet.
Discomfort is frequently worse at the start of activity, eases as the body warms, then lingers later the same day or the following morning.
In Spa & Massage clinics, therapists note that repeated calf loading—such as stairs or plyometrics—can reproduce tenderness along the inner shin, especially when a shoe change coincides with new training.
Likely Underlying Causes
In most cases, the pain pattern labelled “shin splints” reflects medial tibial stress syndrome arising from repetitive tibial loading that outpaces the lower leg’s capacity to recover.
Common drivers include sudden increases in running volume, hills, speed work, or harder surfaces, plus inadequate rest between sessions. Biomechanical contributors may involve overpronation, limited ankle dorsiflexion, and reduced hip stability, which increase traction through the tibialis posterior and soleus onto the tibial border.
Calf tightness and myofascial overload can heighten local sensitivity and perceived “pulling” along the inner shin.
Footwear with poor support or worn cushioning, and low bone-density risk factors, can also raise stress.
At Spa & Massage, therapists screen for red flags and refer for assessment if focal bone tenderness suggests stress fracture.
When It Isn’t Safe (Red Flags)

It is not appropriate for shin pain with severe swelling, rapidly escalating pain, or inability to weight-bear, as these features can indicate pathology beyond medial tibial stress syndrome.
If a stress fracture, acute muscle tear, or tendon rupture is suspected, Spa & Massage therapists advise pausing treatment and seeking prompt clinical assessment and imaging where indicated.
Massage is also contraindicated when symptoms suggest blood clotting or infection (for example, unilateral calf warmth/redness, fever, or spreading skin changes), because tissue manipulation may increase risk and delay urgent care.
Severe Pain Or Swelling
When should severe shin pain or swelling be treated as a red flag rather than something to “work through” with massage?
If pain is intense at rest, worsening day to day, or paired with rapidly increasing swelling, heat, redness, or marked tenderness along the shin, deep tissue work is not appropriate. These signs can indicate an acute inflammatory flare or a circulation-related concern where pressure may aggravate symptoms.
At Spa & Massage, therapists screen for visible swelling, pitting, and pain that alters gait; if present, they pause treatment and recommend prompt clinical assessment.
Massage should also be deferred when swelling is accompanied by numbness, tingling, or a feeling of tight, expanding pressure in the lower leg. Gentle, non-compressive comfort measures are safer until reviewed.
Suspected Fracture Or Tear
How can a clinician distinguish routine shin-splint soreness from a suspected stress fracture or soft-tissue tear where intensive tissue massage becomes unsafe? Red flags include focal, pinpoint bone tenderness, pain that persists at rest or at night, pain with hopping, or swelling/bruising after a single “pop” or sudden change of direction.
A tear is more likely when pain is sharp, immediate, and accompanied by weakness or loss of function; a stress fracture is suspected when impact loading rapidly worsens symptoms despite rest.
In these scenarios, Spa & Massage therapists would not apply deep tissue pressure over the shin or calf and would advise prompt clinical assessment and imaging if indicated. Gentle, non-compressive comfort work away from the site may be considered only with medical clearance.
Blood Clots Or Infection
Given the potential for serious complications, clinicians treat suspected deep vein thrombosis (DVT) or infection as clear contraindications to deep tissue work for shin pain.
Red flags include new unilateral calf swelling, warmth, tenderness, visible vein distension, unexplained shortness of breath, or risk factors such as recent immobility, surgery, or hormonal therapy.
For infection, watch for spreading redness, fever, chills, escalating pain, or a hot, shiny area, especially after skin breaks.
Deep pressure may dislodge a clot or worsen tissue spread, so urgent medical assessment is required.
At Spa & Massage clinics across London, therapists pause treatment and advise same-day GP, NHS 111, or emergency care, then resume only once cleared, offering gentle, non-compressive comfort elsewhere.
How It Can Ease Shin Splints
In cases of shin splints (medial tibial stress syndrome), intensive tissue massage may help reduce pain by targeting overloaded calf and tibialis posterior/anterior tissues that contribute to traction and stress along the tibial border. By easing myofascial tension and trigger points, pressure on the periosteal attachments can lessen, improving comfort during walking or running.
Massage may also support local circulation and fluid exchange, which can help settle post‑exercise soreness and stiffness.
Clinically, this approach is best viewed as adjunctive care: it may improve tissue tolerance, ankle mobility, and perceived pain, but it does not replace graded loading, footwear review, or rest when symptoms flare.
At Spa & Massage clinics in London, clients often report a calmer, warmer lower leg and easier stride after sessions.
Our Deep Tissue Techniques for Shin Splints

Often, deep tissue work for shin splints is structured around a clinically informed sequence that reduces traction stress along the tibial border by addressing overload in the gastrocnemius–soleus complex and the tibialis posterior/anterior, while respecting symptom irritability.
At Spa & Massage clinics, therapists typically begin with slow, warming strokes to assess tone, then apply sustained, tolerable pressure to the calf aponeurosis and deep posterior compartment, following pain-free tissue glide rather than “digging” along the shin.
Cross-fibre and longitudinal stripping may be used around the soleus and flexor attachments to improve load transfer.
Gentle myofascial release to the anterior tibialis and peroneals supports balanced tension.
Work is paired with comfortable ankle mobilisations and calming breath cues to keep the nervous system settled.
How Many Deep Tissue Sessions for Shin Splints?
For most cases of shin splints (medial tibial stress syndrome), the number of intensive tissue massage sessions is best determined by symptom irritability, training load, and how quickly calf and lower‑leg tissue sensitivity settles between appointments.
In practice, many clients do well with 3–6 sessions, initially spaced weekly, then tapered as tenderness along the tibial border and calf tone normalise.
More irritable or long‑standing cases may require 6–8 sessions, while mild, recent-onset symptoms may settle in 2–4.
A useful benchmark is a clear, measurable drop in pain with palpation and hopping, plus improved ankle dorsiflexion and reduced post‑run tightness.
At Spa & Massage, therapists reassess each visit and keep pressure intimate, focused, and tolerable.
Between Intensive Tissue Massages: Shin Splints Care
Between deep tissue appointments, shin splints care should prioritise lowering tibial load while maintaining lower‑leg capacity, since symptom flare-ups are most commonly driven by cumulative running impact, calf–soleus tightness, and limited ankle dorsiflexion.
Relative rest is preferred: reduce running volume, avoid hills and speedwork, and use low‑impact cardio to stay conditioned.
Daily calf and soleus stretching plus ankle dorsiflexion mobilisations can ease tension; add gentle tibialis posterior and anterior strengthening, progressing only if pain settles within 24 hours.
Supportive footwear and temporary arch support may reduce strain, alongside soft‑tissue self‑massage to calves (not directly on the tender shin).
In Spa & Massage clinics, therapists often suggest warm baths, hydration, and sleep to improve tissue recovery and comfort.
When Shin Splints Need Physio or a GP Checkup?
When should shin splints be assessed by a physiotherapist or GP rather than managed with rest and massage alone? Assessment is advised if pain is focal (one small spot), sharp, or worsens with hopping; if there is night pain, swelling, redness, warmth, numbness, or calf tightness suggesting nerve or compartment issues.
Review is also indicated when symptoms persist beyond 2–3 weeks of load reduction, or recur quickly on return to running, as stress reaction or stress fracture must be ruled out. A physiotherapist can guide graded loading, gait and footwear review, and strength work for tibialis posterior/soleus.
At Spa & Massage, therapists can support comfort with deep tissue and sports massage, but will recommend medical review when red flags appear or progress stalls.
Conclusion
It may help shin splints by reducing calf and tibialis muscle tension, improving tissue glide, and settling pain sensitivity, particularly when symptoms are linked to training load and lower‑leg tightness. It is not a standalone fix and should sit alongside graded load management, calf/foot strengthening, and mobility work. Red flags—night pain, focal bony tenderness, swelling, or worsening with rest—need medical review. Used appropriately, it can be one tool in the toolbox.