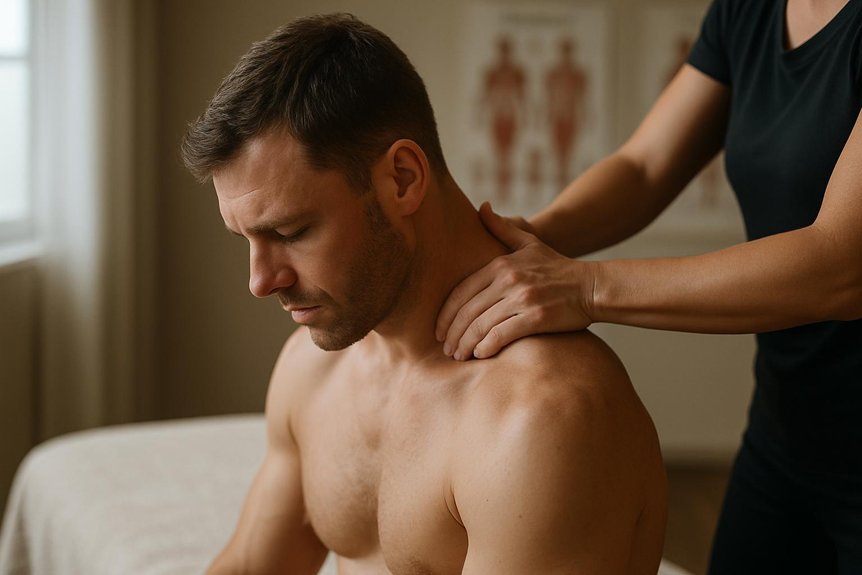
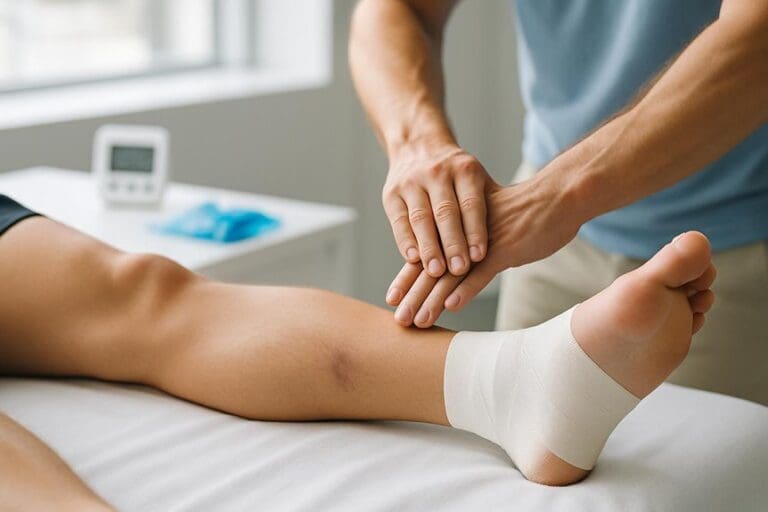
It can help many cases of lower back pain by reducing muscle tension and protective guarding, improving local circulation, and restoring more comfortable short-term movement, especially when paired with sensible loading and mobility. Techniques such as graded pressure, slow strokes, and myofascial release often target the lumbar muscles, glutes, and hips to reduce strain on the back. It will not fix disc-related nerve compression, and red-flag symptoms require medical assessment. Further details clarify who benefits most and what to expect.
Can Sports Massage Help Lower Back Pain?
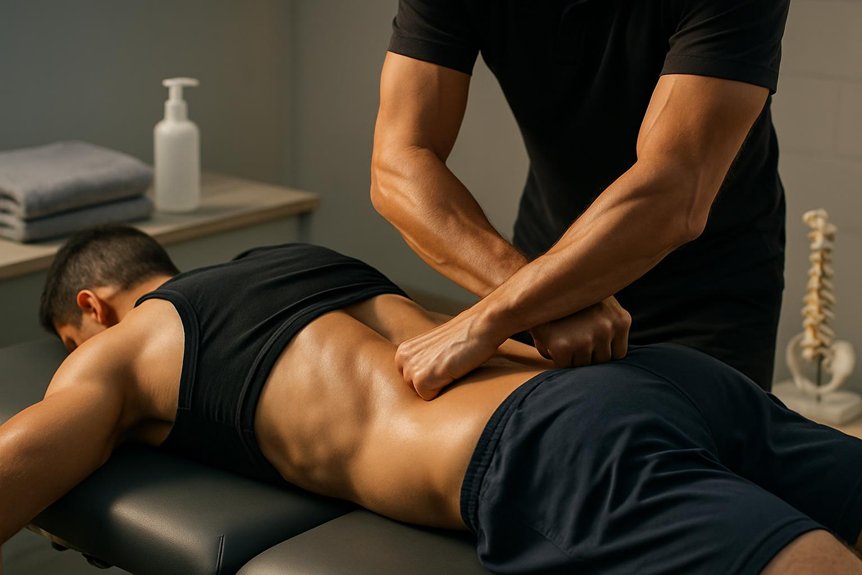
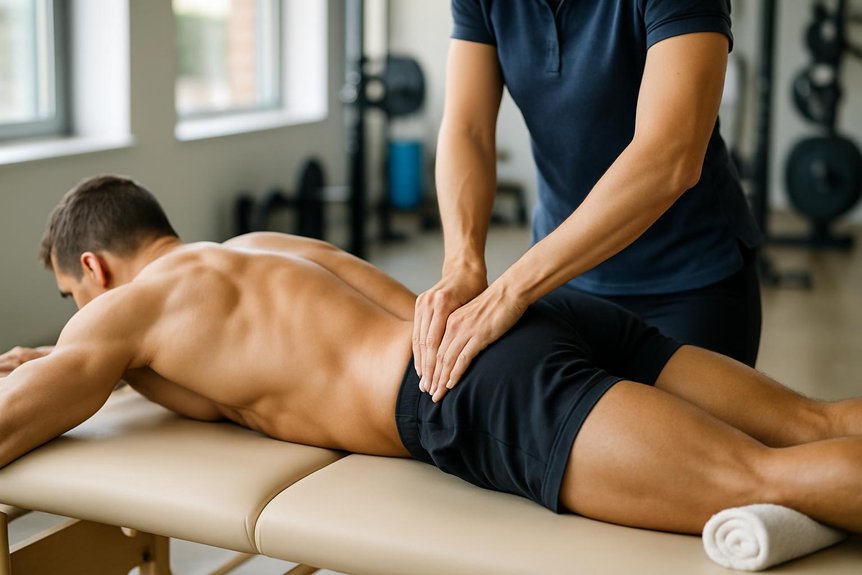
In many cases, athletic massage can help lower back pain by reducing muscle tension, improving local circulation, and restoring more comfortable movement patterns, particularly when symptoms are linked to overuse, postural strain, or soft-tissue tightness rather than serious underlying pathology.
Evidence suggests hands-on soft-tissue work may ease pain sensitivity, improve short-term range of motion, and support faster return to valued activity when paired with sensible loading.
It is widely used among athletes for injury prevention and performance support, which can be relevant when lower back discomfort stems from training load and muscle overuse.
At Spa & Massage clinics across London, therapists assess comfort, irritability, and goals, then tailor pressure and technique—often combining deep tissue and sports methods with slower, reassuring pacing.
Many clients appreciate targeted work through glutes, hips, and lumbar fascia, followed by gentle stretching advice, hydration, and heat/ice guidance.
Persistent pain, night pain, weakness, or numbness should prompt medical review.
What Causes Lower Back Pain in Active People?
In active people, lower back pain commonly reflects a combination of overuse from rapid increases in training load, muscle imbalances or weakness that reduce spinal and pelvic stability, and inefficient movement patterns or sustained poor posture.
These factors can increase tissue stress and sensitise pain, particularly during running, lifting, or prolonged sitting between sessions.
At Spa & Massage clinics across London, therapists assess training habits, key strength and flexibility deficits, and posture to help identify likely contributors and guide practical next steps.
Overuse And Training Load
Under the cumulative stress of frequent training, the lower back can become painful when recovery time is insufficient for muscles, fascia, and spinal joints to adapt. Rapid increases in mileage, intensity, or lifting volume can exceed tissue capacity, provoking irritation, protective muscle spasm, and stiffness, especially after repeated flexion, extension, or rotation. Fatigue also reduces movement quality, increasing spinal loading late in sessions.
Early signs include dull ache after workouts, morning tightness, or pain that escalates across the week.
At Spa & Massage clinics, therapists take a detailed training history and use athletic massage to calm sensitised tissues and support circulation, while encouraging pacing, planned rest days, sleep, hydration, and gradual progression. Persistent pain or neurological symptoms merit clinical assessment.
Muscle Imbalances And Weakness
Even when training load is well managed, lower back pain in active people commonly stems from muscle imbalances and weakness that alter lumbopelvic control and increase stress on spinal joints and soft tissues. Typical patterns include underactive deep core stabilisers (transversus abdominis, multifidus) alongside dominant hip flexors, hamstrings, or erector spinae, creating compensatory bracing and fatigue.
Gluteal weakness may reduce hip extension power, shifting force into the lumbar region during running, lifting, or cycling. Research supports targeted strengthening and motor-control retraining to reduce recurrence, alongside addressing myofascial tone.
At Spa & Massage clinics, therapists assess how tension and tenderness distribute through the hips, abdomen, and lower back, then use athletic massage and deep tissue work to relieve protective guarding, improving comfort so clients can rebuild balanced strength safely.
Poor Movement And Posture
Across many training styles, poor movement mechanics and sustained postural loading are frequent drivers of lower back pain in active people, particularly when fatigue or sport-specific habits encourage lumbar overextension, flexion, or rotation.
Repeated “hinging” from the spine instead of the hips, bracing inconsistently, and collapsing into anterior pelvic tilt can increase shear and compressive stress on lumbar tissues.
Long cycles of sitting between sessions may further stiffen hip flexors and reduce glute contribution, making the back work harder during running, lifting, or sport.
At Spa & Massage, therapists often note protective muscle guarding around the lumbar erectors and quadratus lumborum when posture feels unsafe.
It can calm tone and improve body awareness, but lasting change typically comes from cueing, mobility, and graded strengthening, tailored with care.
Who Should (and Shouldn’t) Get Athletic Massage?

Choose athletic massage when lower back pain is linked to muscular overuse, training load, or persistent soft‑tissue tension that limits movement. It suits runners, gym‑goers, desk workers with guarded lumbar muscles, and anyone returning to activity after a flare‑up, especially when pain is mechanical and eased by gentle movement.
At Spa & Massage clinics across London, therapists tailor pressure and positioning to comfort, using clear consent and ongoing check‑ins to keep the work both effective and close to the client’s boundaries.
Athletic massage should be avoided or delayed with red‑flag symptoms (fever, unexplained weight loss, night pain), new bowel/bladder changes, progressive leg weakness, suspected fracture, infection, cancer, or acute inflammatory conditions.
It is also unsuitable over open wounds, fresh bruising, or untreated blood‑clot risk. Seek medical advice first.
How Does Athletic Massage Loosen a Tight Lower Back?
For those without red-flag symptoms, athletic massage can help a “tight” lower back by targeting the soft-tissue drivers of protective guarding—typically increased muscle tone, local trigger points, and reduced glide between muscle layers and surrounding fascia. At Spa & Massage, therapists use graded pressure and slow, specific strokes to calm sensitised tissues and encourage more comfortable movement.
Clinically, the goal is not to “put something back in,” but to improve circulation, reduce nociceptive input, and restore normal tissue sliding. Techniques such as myofascial release, trigger-point work, and hip–glute integration can reduce the pull on the lumbar area and make standing, bending, and walking feel easier.
Many clients notice immediate warmth and release, followed by longer-lasting changes when sessions are paired with gentle mobility and hydration advice.
Athletic Massage and Sciatica: What It Can’t Fix
Although athletic massage can ease muscular tension around the pelvis and lower back, it cannot resolve true sciatica when symptoms are driven by nerve-root irritation or compression (such as from a lumbar disc herniation or spinal stenosis).
In these cases, massage may temporarily reduce guarding in the glutes, piriformis, and paraspinals, but it cannot “move” a disc, widen a narrowed canal, or calm an inflamed nerve root.
Persistent leg pain, pins-and-needles, numbness, or weakness needs medical assessment, especially if symptoms worsen, night pain appears, or bladder/bowel changes occur.
At Spa & Massage London clinics, therapists screen for red flags and use gentle, comfort-led work only when appropriate, helping clients feel soothed while encouraging timely referral to a clinician.
What to Expect in a Lower Back Athletic Massage
Often, a lower back athletic massage begins with a brief clinical-style intake: the therapist reviews symptom location and behaviour (what provokes or eases pain), relevant training or work loads, prior injuries, and any red flags, then explains a consent-led plan.
In Spa & Massage clinics, the client is positioned comfortably, with draping and privacy maintained, and pressure is agreed throughout. Treatment commonly starts with slow, warming strokes, then targeted deep-tissue and myofascial techniques to lumbar paraspinals, glutes, hip rotators, and hamstrings, as tolerated.
Therapists may include gentle joint mobilisations and guided breathing to reduce guarding and improve body awareness. Sensations should feel “strong but safe,” never sharp, burning, or shooting.
Afterward, brief advice may cover hydration, heat or cold use, and simple movement to sustain relief.
How Many Athletic Massages for Lower Back Pain?
In clinical practice, the number of athletic massage sessions needed for lower back pain depends on the underlying driver (e.g., muscular overload, myofascial restriction, or training-load mismatch), symptom irritability, and how consistently symptoms improve between visits.
For recent, mild flare-ups, many clients feel meaningful change within 1–3 sessions, typically spaced 5–10 days apart to allow tissues to settle and the nervous system to downshift.
With persistent pain or recurrent tightness, a short course of 4–6 sessions may be more realistic, with reassessment each visit.
At Spa & Massage, therapists track tenderness, range, and ease of daily movement; if improvement plateaus after 2–3 well-matched sessions, they advise a clinical review to rule out non-muscular contributors and coordinate care safely.
Aftercare to Stop Back Pain Returning
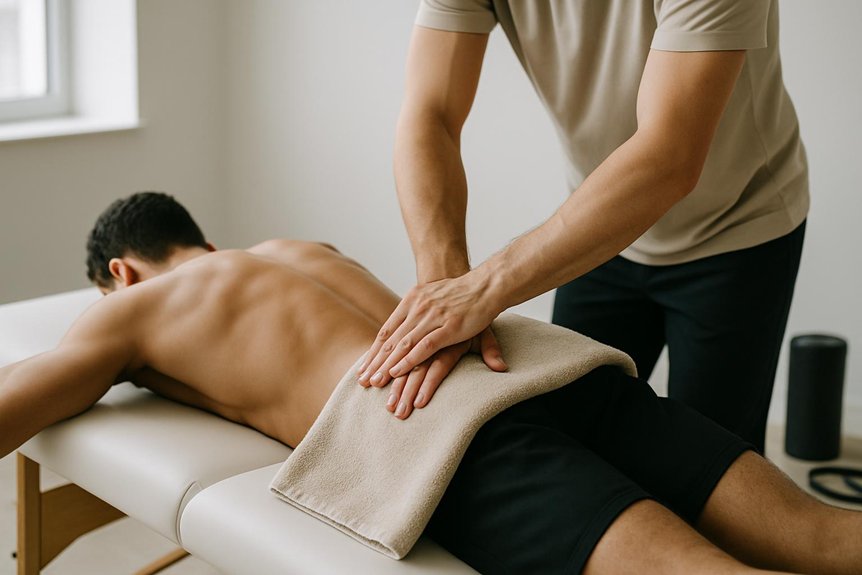
After athletic massage for lower back pain, outcomes are more likely to last when clients follow a simple aftercare plan focused on daily mobility and stretching, alongside consistent posture and movement habits.
At Spa & Massage clinics across London, therapists typically advise brief, regular mobility work and targeted stretches, plus practical adjustments to lifting technique and workstation ergonomics to reduce recurrent strain.
The following points outline how these measures can support tissue recovery, improve load tolerance, and lower the risk of symptoms returning.
Daily Mobility And Stretching
Consistently practising gentle daily mobility and stretching helps reduce recurrence of lower back pain by maintaining lumbar and hip range of motion and lowering tissue stiffness between athletic massage sessions. At Spa & Massage, therapists encourage short, regular sessions that feel soothing, never forced or sharp.
A practical routine includes diaphragmatic breathing with pelvic tilts, knee-to-chest holds, cat-cow, and a supported child’s pose. Hip mobility is often paired with glute bridges and a light hamstring or hip-flexor stretch, held 20–30 seconds, 1–3 rounds. Evidence supports graded movement and calm exposure to comfortable ranges to reduce sensitivity and improve confidence.
If symptoms flare, intensity is reduced, breaths slowed, and heat or a gentle walk added. Persistent numbness, weakness, or night pain warrants clinical review promptly.
Posture, Lifting, And Ergonomics
Daily mobility work is most effective when paired with simple changes to how the back is loaded throughout the day. Neutral spine is helpful, but “perfect posture” is unnecessary; regular micro-breaks, varied positions, and supported sitting often reduce symptom flare-ups.
For desk work, Spa & Massage clinicians advise screen at eye level, elbows near 90°, feet grounded, and a gentle ribcage-over-pelvis stack to keep breathing easy. When lifting, the safest pattern is close-load handling: brace softly, hinge at hips, bend knees as needed, keep the object close, and avoid twisting under load—turn the feet instead.
If pain increases beyond mild discomfort or lingers, workload should be reduced and technique reviewed with a therapist.
Conclusion
Athletic massage may ease lower back pain by releasing guarded tissues and restoring movement through the hips, glutes, and lumbar fascia. Like smoothing a tightened sail, targeted pressure can reduce stiffness, improve range of motion, and support safer patterns of loading. It cannot correct nerve compression or serious pathology, and persistent, spreading, or worsening symptoms warrant medical assessment. With appropriate screening, a short treatment series and clear aftercare may help sustain calmer, more resilient movement.